|
ATOPIC DERMATITIS
|
|
|
|
Atopy : is a genetic predisposition to form excessive IgE antibodies. The reaction may manifest with one or more of immunologic reaction such as eczema, asthma, hay fever, and conjunctivitis. In 1925 Coca introduced the term "Atopy" to signify the tendency to develop allergies to food and inhalant substances as manifested by skin reaction, asthma and hay fever on a hereditary bases. Atopic dermatitis is considered by some authors as: atopic eczema, allergic eczema, infantile eczema, disseminated neurodermatitis. Specific Features of Atopic Dermatitis Atopic persons have certain specific features:
Different Clinical Types of Atopic Dermatitis The clinical manifestation and management of atopic dermatitis varies according to the different age groups. Atopic dermatitis may be divided according to the age of onset into three types:
INFANTILE ATOPIC
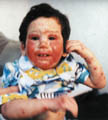
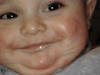
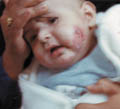
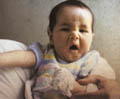
DERMATITIS Infantile eczema is the most common form of dermatitis which begins usually before the age of six months or may appear later in childhood or in adult age.It is estimated that more than 3% of infants and about 25% of children are affected between the age of three and twelve years.
Skin manifestations appear after birth between two months to two years of age. In atopic dermatitis there is usually a hereditary predisposition with a familial history of atopy with urticaria, hay fever or asthma. Etiology Different factors have an important role in the etiology of infantile eczema.
in the majority of cases. The most common foodstuff that may exacerbate or initiate atopic dermatitis are: Ingestants such as milk, egg white, wheat, cereals, orange. Food allergy should be suspected in infant who manifests with regurgitation of food, vomiting and colic after feeding. Food coloring or other additives such as tartrazine may also have an important role.
Exacerbating factors Exacerbation of the eczematous lesion may be due to:
N.B.
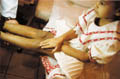
Skin manifestations The distribution of the skin lesion is not always characteristic in infants. Skin lesions affect cheeks, neck, flexural, popliteal areas and antecubital areas. Erythematous patches appear with minute vesicles, which later become moist oozing and crusted lesions. Secondary infection that is presenting with pustules and crusts is very common, predisposed by the abraded skin surface and severe itching. The infant becomes irritable, always crying and rubbing his skin severely. This vicious circle of itching-excoriation may lead to more complications after healing such as skin scarring. The skin lesion may extend to involve the cradle cap area and the scalp presenting with crusted oozing vesicular patches. Systemic manifestations Erythroderma and constitutional symptoms such as fever, vomiting, abdominal colic and diarrhea are common in severe cases of infantile eczema. Immunologic abnormalities in atopic dermatitis
Course of infantile eczema The course is variable but usually the lesion improves or even disappears by the end of the second year. There is a tendency of recurrence in childhood or later in the adult age, where the manifestations are less severe and dry. Diagnosis of Infantile Eczema The clinical picture and the distribution of lesions are characteristic. Skin tests may be misleading and give false reactions in the early age groups. These tests are usually positive after the fourth month of age and should not to be requested routinely. They are expensive, unreliable, embarrassing for the infants and sometimes give false reactions. Certain foodstuff may be eliminated from the infant meal according to these tests which may be crucial for his growth.
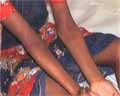
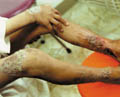
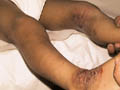
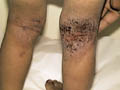
This clinical type of atopic dermatitis is present in children after the fourth year of age. The lesions are usually less acute than that of the infantile type of atopic dermatitis. The lesions in childhood eczema are mainly eczematized, excoriated and may be lichenified. A very characteristic feature of this type of eczema is its tendency to spread far from its point of origin, especially when the primary site of the eczema is on the legs or the feet. Dissemination is often preceded by an exacerbation by inflammation at the primary site. Clinical manifestations Eczema in childhood is less acute. Oozing is less and the lesions are usually dry. The primary lesion is erythematous acutely inflamed. The eruption increases in severity and may be accompanied by generalized erythema and exfoliation of the skin surface.
The most common sites involved are the ante-cubital, popliteal fossa, wrist and around the neck.
Lichenifecation and scaling due to continuous scratching is a predominant feature in childhood eczema. The secondary eruption first presents with small edematous papules. These soon become obviously eczematous, grouped papulovesicles, which may become confluent in small plaques. Occasionally the lesions take the form of red macules or wheal and usually have a symmetrical distribution. The course of the secondary eruption depends largely on the progress of the primary lesion. Dissemination may occur due to contact with an external allergen, ingestion or injection of an allergen or conditioned hyper-irritability. Heavily infected eczema will sometimes disseminate in the absence of demonstrable allergic sensitivity to topical medicaments. It is probable that allergy to bacteria or their products sometimes play an important factor in the dissemination of eczema. Sensitizers in childhood eczema Sensitization by foodstuffs such as milk, egg white and wheat is less in childhood atopic dermatitis. There is an increased liability to sensitization to inhalants in childhood with pollens and contact with wool, animals such as cats and dog‘s hair. Sensitivity to wool is the most common and this explains the recurrence of the eczematous lesions each winter. Sensitization to different materials such as metals in jewelry, ragweed is more in atopic patients than in normal individuals. Treatment of Infantile and Childhood Atopic Dermatitis Topical and systemic medications should be used with much care in the young age groups. Toxins and chemical ingredients included in the topical preparations may be easily absorbed from the abraded skin surface adding more unwanted side effects. There is nothing that destroys the confidence of the atopic patient more than prescribing medications which were used by the patient and proved to be ineffective. It is wise before prescribing any medication to ask thoroughly about other medications used by the patient. General measures Atopic dermatitis when handled in a proper way can be easily controlled. In most cases the skin problem usually disappears towards the end of the second year or even before. The mother should have a thorough idea about atopic dermatitis, causes, prognosis and exaggerating factors. Bathing The skin of infants and children is very sensitive and the physiochemical properties of their skin should be kept within the optimum conditions. The child‘s skin is thinner than that of adults, skin furrows are less deep and have more vellus hairs, which keep the cutaneous follicles more open.
The sebum on the surface of the infants skin begins to decrease in the first few months. These factors will lead all to increase in the susceptibility to infection, increased permeability and sensitivity to detergents and other toxic substances. The skin has an acid pH (Potential Hydrogen) which ranges from 4.2-5.6. The pH is measured on a scale ranging from 0 to 14. The center of the scale, 7, is neutral (neither acid nor alkaline). A reading above 7 indicates that the substance is alkaline, below 7, is acidic. The pH varies from one part of the body to another and according to the age and sex (The pH of males is more acidic than females). That plays an important role in skin-surface bacteriostasis. Strong acidic or alkaline soaps or shampoos especially those containing perfumes or coloring chemicals may revert the pH of the skin surface and may cause more dryness of the skin predisposing to eczematization or infection. The skin of infants and children needs usually only gentle cleaning with "non soaps " which is synthetic detergents and applying mild natural or synthetic emollient. Mild emollients are saturated triglycerides, long chain alcohol (stearyl, cetyl) or polyethylene glycol or glycosaminoglycan products. The normal child should take a bath once every two days. The period of bathing should not take more than 5 minuets for an infant and not more than 10 minuets for a child. The napkin area can be cleaned gently when required with mild soap and drying of the area better with soft cotton towels, cloth or with soft tissue paper free of perfumes. Vegetable oils such as olive oil or petroleum jelly can be added in case when the skin is dry. Perfumed foam bath should not be used, Potassium permanganate solution1: 9000 may be added as an antiseptic in infected skin lesions or bran extract to very sensitive skin or an emollient. Cleansing of the newborn should be in a gentle and non-traumatic way. It is important not to use harsh and strong shampoo but the scalp can be cleansed by very mild baby shampoo. Cradle cap in the newborn can be washed easily . If the layers of crust are thick, these can be removed using warm vegetable oil such as warm olive oil soaks to the area and then very gently combed. Children have protective lipids less than those of adults, so cream soaps are recommended especially those containing emollients as well as non-soap preparation. In short the soaps used for infants and children should have the following properties:
Bathing of the newborn and infants especially in cases with atopic dermatitis should be gentle using a soft sponge. Rubbing or using plastic or harsh sponges may lead to more excoriations, irritation and itching. Different ingredients may be added to the bath according to the type of the skin lesion. Antiseptic solution such as potassium permanganate 1: 9000 may be used for infected cases. Emollient baths: prepared with olive or other plant oils can be used for the dry skin lesions. Emollient baths are used to lubricate dry skin lesions. These are mainly lanolin, liquid paraffin or mineral oils as olive oil. Care should be taken not to keep these emollients for a long time on the skin because of possibility of their occlusion of the skin surface encouraging anaerobes to grow on the occluded skin surface or cause sweat retention Colloid baths - are soothing baths used for itchy skin lesions and can absorb hydrophilic and lipophilic substances. Colloid baths are powders, as oatmeal should be mixed well with water in order not to cake causing more abrasion to the child‘s skin. The type of soap or shampoo used for infants and children should be mild and has "tensid," a substance having the characteristic of hydrophilic and lipophylic property leading to gentle cleaning of the skin surface. Cleaning of the skin can be safely done with gauze soaked in olive oil especially if the area is dry. Clothing: overheating the skin of the infant by heavy clothing is not always recommended . In cold weather, moderate dressing is recommended. If there is any doubt that woolen clothes cause flare up of the condition, cotton long sleeve and trouser dressings should be worn under the woolen ones. Care should be also taken concerning socks. Woolen or polyester socks may cause exacerbation of the skin lesion. Jewels - gold, nickel, chromate and other metals can cause contact dermatitis. Sodium chloride in the sweat may combine with the metal and may cause contact dermatitis and black discoloration with silver jewels. Infant bedroom: Woolen or feather pillows and covers should be avoided due to possibility of sensitization. The floor of the bedroom is preferred to be of tiles or wood. Carpets, indoor plants and roses are better avoided in the infant‘s bedroom. Pets: dogs, cat, birds, and rabbits should be kept away. Feeding: over feeding is not recommended. Eczema due to foodstuffs usually begins during the first year. Routine elimination of eggs, wheat (cereals), juices or changing breast-feeding to bottle feeding is considered as unwise step unless there is strong supporting data that such type of food is confirmed to trigger and precipitate an allergic reaction. When foodstuffs are blamed as a causative factor, skin test can be considered. Milk, eggs and wheat are the most common. Food substitute for milk is soya beans emulsion, for wheat, oatmeal, boiled rice, soya bean flour or corn flakes. Fondling of the atopic infant may sometimes exaggerate his skin problem as by the cosmetics such as that of the lipstick, make up or by the moustache or scalp hair. Perfumes: these are better applied to the external clothes before dressing the infant. Liquid perfumes are preferred instead of spray perfumes especially in very sensitive infants.
Topical medications The most important line of treatment in atopic dermatitis is to relieve itching. Covering the hands of the infant by cotton gauze or using special cotton gloves besides topical and systemic preparations Topical preparations Oozing wet eczema should be dried by Potassium permanganate 1: 9000 compresses. Sterile gauze soaked in the solution applied gently on the area for several times avoiding harsh or vigorous rubbing. Lotions are used for the oozing surface. Creams are applied for subacute cases that are less wet. Ointments containing mild corticosteroid (Elocom) can be applied for the dry lesi Non-steroidal topical preperations are the first line of treatment in infantile atopic dermatitis.Corticosteroids should be reserved for the most severe,reluctant types of atopic dermatitis when the non-steroidal preperation fail to clear the lesions. The most effective and safe antisteroidal topical preperations are Pufexamac ( Droxaryl or Flogocid )andTacrolimus (Protopic cream). Immunomodulating agents There is a continual search in dermatology for more selective anti-inflammatory drugs to replace broad spectrum steroids. Tacrolimus (FK506), which is related to cyclosporin, is a powerful immune suppressor that was introduced to reduce organ transplant rejection. Like cyclosporin, it has been used systemically to treat psoriasis, atopic dermatitis, and pyoderma gangrenosum. Unlike cyclosporin, tacrolimus seems to be effective when applied topically. Initial open trials suggest that over 90% of children and adults rapidly achieve at least good improvement of atopic dermatitis. There is no systemic accumulation. Adverse effects occur in about half but are transient and are predominantly burning and erythema at the application site Tacrolimus (Protopic cream): is a non-steroid topical preperation .This is safe and effective in eczematous skin condition mainly atopic dermatitis.The drug prooved recently to be effective in vitilligo.Tacrolimus ointment is a steroid-free topical immunomodulator developed for the treatment of atopic dermatitis, a common, chronic inflammatory skin disease. By inhibiting T-cell activation and cytokine production, topically applied tacrolimus modulates inflammatory responses in the skin. Numerous clinical trials have shown that it is effective and well tolerated for the treatment of atopic dermatitis, its licensed indication. In addition, numerous publications suggest that tacrolimus ointment may provide effective treatment for a variety of other inflammatory skin disorders, many of which are very difficult to manage with standard therapy. Fluorinated or potent steroids should be avoided. If the area is infected, a combination of steroid and antibiotics such as Gentamycin or Sodium Fucidate (Decoderm or Fucicort) is recommended for few days. Topical preparations may loose their efficacy when used for a long time or when applied repeatedly by the patient. This may be due to an acquired resistance against the ingredients or due to a psychogenic factor, where the patient or his family looses faith in that preparation because it couldn‘t cure the condition dramatically and permanently. Topical preparations containing anti-histamine, Neomycin, Sulfa or Penicillin medications should not be used due to the possibility of local sensitization especially when used for prolonged periods. Systemic medications Antibiotics: systemic antibiotics can be given if there is secondary bacterial infections, which usually accompany most excoriated eczematized lesions. Erythrocin, Zithromax or Cephalosporin are effective medications. It should be noted that Cephalosporin has cross reactivity with Penicillin and there fore should not be given to patients sensitive to penicillin. Corticosteroids: Oral or parental corticosteroids are given under strict conditions for infants and young children. All possible medications should be given first before planning to give systemic corticosteroids for these young age groups. Antihistamines: antihistamines whether in drops or in syrup form can be given to relieve itching. Extra care should be taken into consideration to adjust the optimum doses and to use the suitable and a safe antihistamine. It is of prime importance to instruct the mother to abide strictly with the instructions concerning doses in order not to abuse, misuse, repeat or change medications, unless indicated by the treating physician. Skin lesions usually need time to clear and respond to medication. Therefore the family of the patient should have reasonable patience. Shifting from one clinic to another may do more unwanted side effects where some physicians may give potent unnecessary medications to prove that they are more experienced than those previously consulted by the patient and that will be a greedy act on the expense of the patient‘s health.
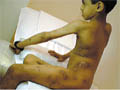
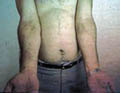
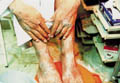
Atopic dermatitis in these age groups is less acute and affecting usually the sites involved during the childhood. The main immunological abnormalities are excessive formation of IgE with a predisposition to anaphylactic sensitivity and some decrease in delayed cell-mediated hypersensitivity. Different sensitizing agents may have an important role in adult atopic dermatitis, and can be detected by skin tests or by exclusion methods. Such types of foods may include the following : Dairy products, eggs, seafood, wheat, nuts, beverages as coffee, tea, lemon, mango, strawberry, canned foods and many others. Coloring and preservatives of food may have an important role. Nervous tension, stress and continuous fatigue are important predisposing factors for atopic dermatitis. Atopic patients are more susceptible to respiratory tract, viral infections, and eye complications as lens opacity and cataract. General Features of Adult Atopic Dermatitis The clinical picture tends to be localized and drier. The skin lesions are usually localized pruritic and lichenified patches that present as erythematous scaly excoriated and with well demarcated edges. The patches involve mainly the neck, flexures, popliteal and antecubital fossa. Pruritus is severe in some cases that may lead to more excoriation of the lesions and predispose to secondary bacterial infection. Clinical Manifestations Skin lesions varies from papular, vesicular, erythematous or dry lichenified pruritic patches, affecting the front and sides of the neck, forehead, wrists, hands, antecubital, popliteal and the lower limbs. Skin lesions may become confluent forming dry, lichenified, hyperpigmented plaques. Severe scratching is the main distressing symptom, which may cause more exaggeration and complication, leading to sweat retention, secondary bacterial and fungal infection. Nervous tension and psychosomatic disorders have an important role in exacerbating the condition and increasing the severity of itching. Eye changes: lens opacities Upper respiratory tract infection. Susceptibility to bacterial and viral infections such as herpes labials. Diagnosis Atopic dermatitis can be diagnosed by different criteria mainly:
Management of Adult Atopic Dermatitis
Topical Treatment Atopic dermatitis in adulthood is usually of the dry type so ointments containing mild steroid in an emollient base may be enough to control small-localized lesions. Corticosteroid ointment in combination with salicylic acid (Locosalene, diprosalic) are used for dry lesions. Hydration of the skin is helpful, using non-sensitizing moisturizing preparation especially after bathing or during winter and in dry tropical areas. Cases complicated by secondary bacterial infection require oral antibiotics such as erythrocin and a topical steroid cream combined with antibiotic as Gentamycin with Betamathesone valerate or other fluorinated corticosteroid (Celestoderm v with Garamycin or Decoderm). Local sensitization to lanolin, paraben or topical medications such as topical antihistamine and even corticosteroids may in some cases cause exacerbation of the skin problem. Emulsifying ointment BP (hydrophilic ointment), oatmeal, or bran can be used as substitute to the allergenic base of the topical preparations especially Parabens. Bathing should be minimized using special oily soap free from strong detergents, perfumes or added antiseptics. Systemic corticosteroids: Oral or parental steroids should be reserved for reluctant cases not responding to topical preparations. Oral corticosteroid dose can be given as one dose in the morning or doubled and given every 48 hours .The dose depend on the severity of the lesion, body weight and other factors related to the patient. In adults Intramuscular injection of long acting steroids such as (Depot medrol) 40 mg. weekly for 2-4 weeks is usually more practical and leave no doubt in misusing the scheduled oral doses of cortisone preparations. Triamcinolone intramuscular suspension in a dose of one injection 40 mg. at intervals of 2-4 weeks can also be used, giving good results and minimizing adrenal suppression.
|
| Contents | << Previous Chapter | Next Chapter >> | Search |