|
Diaper dermatitis is an
eczematization of the areas covered by diaper. Continuous occlusion ,
moisture and maceration of the diaper area may cause non-physiological
state, where skin cannot tolerate that indefinitely. Fermentation of the
secretions and liberation of ammonia plays also an important factor. Obese
well-fed infants are more predisposed to have diaper dermatitis .
Etiology
Inspite that different
physiological and pathological factors that play an important role in the
etiology, yet the allergens that can cause the skin lesions in one infant
may be not the same as that in another infant.
Predisposing Factors
-
Maceration of the
crural area: This will lead to changing the optimum physiological status
of the crural area.
-
Occlusion of the
Crural Area: Prolonged occlusion of the skin can itself produce erythema
due to increasel sweating and accumulation of debris on the crural area.
-
Water: Water is an
important irritating factor especially when their contents of salts or
chlorine are higher than the standard or using polluted water.
Hydration and friction
may be responsible for many cases of napkin dermatitis making the skin
more susceptible to irritants. It has been suggested that prolonged
contact with water alone can provoke dermatitis.
Maceration of the stratum
corneum by water may be an important predisposing factor, which increases
transepidermal permeability, friction and infections .
-
Urine
The role of urine in
precipitating the skin lesions may be due to increased pH or higher
contents of ammonia .
Ureas are produced by a
variety of fecal bacteria, which will have the effect of increasing the pH
when mixed with urine.
This may explain the
findings that breast fed infants are less liable to diaper dermatitis than
those fed on cows‘ milk , since the feces of the former group have been
shown to be less heavily colonized by urease-products .
In addition, urine
appears to increase trans-epidermal permeability more effectively than
water alone .
-
Feces
Human feces have an
irritant effect on skin . Infants feces contain substantial amounts of
pancreatic protease and lipase. Similar enzymes appear to be produced
within the gut by a variety of bacteria causing irritation and leading to
higher pH of feces.
One of the factors that
have been shown to affect fecal pH is the infant‘s diet. Higher pH being
found in the cows‘ milk formula-fed infant .
-
Friction
It seems likely that
friction between the skin and the fabric of the nappy plays at least some
part in the etiology .
-
Micro-organisms
The use of broad-spectrum
oral antibiotics increases the recovery of Candida albicans from the
rectum and skin. These may aggravate primary irritant napkin dermatitis.
-
Chemical irritants
Soaps, detergents and
antiseptics used to clean washable napkins have often been incriminated in
the initiation and aggravation of primary irritant napkin dermatitis.
-
Obese infants are mor
susceptible to diaper dermatitis.
We found that diaper
dermatitis is more common in female infants. This may be related to
different mode of urine voiding, ano-genital secreations, concentrated
urine, more susceptable to Candidiasis or due to other factors.
Clinical Features
The onset is most often
during the second and third month .
Skin lesions :
Confluent erythema of the
areas in contact with the diapers i.e. the buttocks, the genitalia, the
lower abdomen, pubic area and the upper thighs. In some infants, the
eruption is more or less confined to the margins of the napkin area.
Napkin dermatitis may present with different clinical manifestations.
Acute lesions: the
erythema may have a glazed appearance, where later , there may be
exfoliation of the affected areas of the skin.
Chronic cases show
finer scaling .
Erythematous type :
Intensely red confluent erythema of the entire perineal area including the
depths of the flexural folds. Skin lesions present with erythema and
slightly elevated margins. Within the marginal area small pustules may
involve the periphery of the erythema - so-called ‘satellite‘ lesions.
This clinical type is
associated with more intense proliferation of Candida albicans and is
invariably associated with fecal carriage of this organism .
|
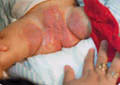
Fig. 175. Diaper Dermatitis |
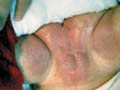
Fig. 176. Diaper Dermatitis
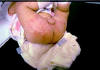
Fig. 176b. Diaper
dermatitis |
Psoriasiform type : the
erythematous areas are similarly well marginated but have a psoriasiform
aspect with prominent scaling. The onset of this eruption is commonly
termed ‘napkin psoriasis‘ that may be quite sudden and its extension
is rapid.
Herpetiform type : This
takes the form of an eruption of vesicles and pustules followed by shallow
erosions, and closely resembling herpes simplex clinically, but showing no
evidence of this infection pathologically.
Granulomatous type : This
rare type manifests with a dome shape , reddish-brown or purple nodules.
The lesions are usually known as infantile gluteal granuloma .
Extensive type : The
lesion extends peripherally to include the lower abdomen and back which
may reach the axillary folds. Some believes that such type is a
manifestation of infantile seborrheic dermatitis .
Hypopigmented type:
Post-inflammatory
hypopigmentation may be a striking feature in racially pigmented infants.
The author found that the
hypo pigmentation was mainly more in infants treated with topical steroids
.
Erosive type of primary
irritant napkin dermatitis is seen, in which small vesicles and erosions
may develop into rather characteristic shallow round ulcers with raised
crater-like edge.
Involvement of the
genitalia may lead to dysurea, if the glans penis is severely affected,
male infants may experience acute retention of urine .
Differential Diagnosis
Candidiasis
Candidiasis has
characteristic clinical features in infants. Skin lesions of candidiasis
are confluent glistening, sharply marginated erythematous with peripheral
desquamation which may be accompanied by pustulation. Satellite pustules
besides oral candidiasis are commn.
In neonatal Candidiasis,
a superficial candida infection is transmitted to the baby during birth .
The rash normally appears during the second week of life.
Congenital syphilis
Congenital syphilis has
to be considered in infants with a dermatitis in the napkin area.
Clinical Features
The lesions of congenital
syphilis appear as reddish-brown macules, sometimes slightly raised which appear principally on the extremities including the palms
, soles, and
on the face mainly around the mouth. The napkin area is also frequently
affected.
|
Bullous or erosive
lesions may occur in the napkin area.
|
|
Flexural condylomata .
|
|
Rhinitis.
|
|
Hepatospleenomegaly .
|
|
Low birth weight is
regular features.
|
Diagnoses
Serological tests (VDRL ,
Treponema palladium immobilization test (TPI) are positive .
The Fluorescent
Treponemal Antibody Absorption test ( FTA-ABS ) is a confirmatory test in
cases of false positive and false negative tests .
This test gives positive
result in almost every case of syphilis .
Zinc deficiency
Zinc deficiency must be
considered in any infant with a napkin dermatitis, which fails to respond
to appropriate treatment. A history of prematurity should increase one‘s
suspicion, and a normal plasma zinc level does not rule out the diagnosis.
Clinical feutures of zinc
deficiency dermatitis
Infants with napkin
eruptions caused by zinc deficiency present with:
Concurrent facial
dermatitis extending from the perioral area.
An erosive paronychia.
Erosions of palmer
creases of the hands.
Histiocytosis
Napkin dermatitis is one
of the most common skin lesions of Langerhan's cell histiocytosis in infants
.
Dermatophytes infections:
Tinea cruris can be differentiated by the active raised edges, central
clearing of lesions and by detecting of the causative organism.
Herpes simplex virus
infection The eruption is acute, has characteristic painful grouped
vesicular lesions on an erythematous base and is accompanied by
constitutional manifestations such as fever .
Treatment of Napkin
Dermatitis
Successful treatment of
napkin dermatitis depends mainly on detection of the predisposing factors.
The application of topical medications alone without correction of the
predisposing factors, usually is rewarded with a therapeutic failure.
1- General measures
-
Washable diapers :
When disposable diapers are not available due to economical or other
reasons , the washable diapers can be used and they are preferred .
Care should be taken concerning the washable diapers in order to give
the best results . These include :
Type of cloth : the cloth
should be made of soft cotton that can easily absorb excretions and should
be free from polyesters .
Absorbency of napkins.
The absorbency of the napkin is another important factor.
Washable cloth napkins
have the advantage of allowing two or more layers to be worn at once in
order to increase the volume of urine that can be effectively absorbed. As
the baby becomes older, though the frequency of urination falls, the
volume voided on each occasion rises.
New diapers should be
washed before using for the first time to sweep away any chemicals .
Washing of the diapers
with mild soap and there should be good rinsing to remove any remnants of detergents .
It is preferred that
diapers are soaked after washing. Few drops of lemon juice or white vinegar
are added to the soaked diapers and left for an hour or more and then washed under
the tap water , rinsed and dried . Diapers should be made of soft cotton
cloth . Harsh and stiff cloth may cause chaffing to the area.
Diaper should not be too
tight , too loose on the skin surface , should not be kept for a long time
and should be changed immediately after wetting .
-
Disposable diapers
are available in the market of different types and with different
efficiency . The mother should use a good quality, which can absorb easily
. She has to take care of the inner lining of the diaper to be free from
plastic or polyester inner lining , which comes in contact with the skin
of the infant. Suitable size of diapens according to the age of infant
should be used in order not to compress the skin of thighs and abdomen.
Care of the napkins
The use of antiseptic
solutions for the storage of napkins prior to washing is more or less
universal. These may be safe as long as suitable agents are used besides washing and
rinsing procedures are adequate. Toxicity of infants by antiseptics used
in the laundery washing of napkins is well documented or due to ink
marking used or related to some detergents ,antiseptics and preservatives
as phenol .
The quaternary ammonium
compounds are now regarded as the best choice, of which benzalkonium
chloride is perhaps the most widely employed. Antiseptics should never be
used during the rinsing process.
Marking inks of the
washable napkins have caused aniline poisoning. These may cause
methaemoglobinaemia when the napkins have not subsequently been washed
before use .
Storage of napkins in
mothballs containing naphthalene has caused hemolytic anemia and fatal
cases among infants .
The mother should pay
more care and attention to her infant . Babies under the care of
housemaids who usually neglect changing the diapers are more susceptible
to develop diaper dermatitis .
Change of diapers
The frequency of napkin
changes is almost certainly more important than either the type of napkin
or the wearing of occlusive pants.
A reasonable plan is a
routine changing or at least checking the napkin for wetting or soiling at
regular periods .
2- Preventive measures
Effective treatment is
directed mainly to prevent the irritating agent and directed towards the
predisposing factors .
Avoid using tissue paper
for cleaning the skin especially those soaked with alcohol, antiseptics or
perfume.
Gentle cleaning of the
diaper area is very important. Mothers should use very mild ,
non-irritating soap and non-perfumed .
Meticulous cleaning will
do more harm .Rubbing the area with a sponge or other harsh sponges should
be avoided .Cleaning by a mild soap and a cotton texture sponge is that
all needed .
At each napkin change, an
emollient such as white soft paraffin, or a half-and-half mixture of white
soft paraffin and liquid paraffin, or zinc and castor oil cream BP should
be applied if the napkin has not been wetted or soiled.
If the napkin has been
wetted or soiled, the area should be cleansed with water and a
water-miscible emollient application such as emulsifying ointment BP,
aqueous cream and dried before applying a water-repellent emollient.
During remission, the
baby should be bathed with dispersible bath oil added to the water, e.g.
Alpha Keri, Oileatum or Balneum, and emulsifying ointment BP, aqueous
cream BP or Unguentum Merck should be used . While the eruption is under
treatment, such baths should ideally be given daily.
The use of talc and
over-the-counter preparations containing potential irritants should be
discouraged.
Cleaning of infants
The ideal cleanser for
new born and infants should have the following features:
Must contain delicate
tensides.
Must be
physio-chemically
stable.
Must not contain perfumes.
Must not contain alcohol.
Must not contain
substances cross-reactive with other allergens.
Must not contain
substances that can be metabolized by cutaneous microflora.
It is important that the
napkin area is left exposed and free for sometime daily without diapers
for aeration .
Rubber plastic panties
worn over the napkin should be avoided or used with care since these may
cause more occlusion.
Powders such as talcum powder
should be avoided if the napkin area is macerated as that may be is
abrasive and may cause more irritation.
3- Active treatment
Non-steroidal
topical preperations : are the first line of treatment
Corticosteroids
should be reserved for the most severe,reluctant types of atopic
dermatitis when the non-steroidal preperation fail to clear the lesions.
The most effective
and safe antisteroidal topical preperations are " Pufexamac
"
( Droxaryl or
Flogocid ) and "Tacrolimus " (Protopic
cream).
Fluorinated or
potent steroids should be avoided.
Topical
antihitamines should not be used.
Treatment depends on the
type of the lesion of the diaper area .
Oozing lesion: Potassium
permanganate 1: 9000 compresses are used to dry the lesion . Clean or
sterile gauze immersed in Potassium permanganate is used as compresses
applied gently to the oozing surface for one minute, and this can be used
frequently.
The physician should be
very careful in choosing the topical preparations because of the
possibility of local sensitization by some creams or lotions containing
sensitizers such as neomycin, local anesthetics ,antibiotics ,
antihistamine preparations and others. The area is scalded and the
possibility of rapid absorption of toxins and others as potent
corticosteroids may endanger the life of the infant.
Topical corticosteroids
Although
some physicians use corticosteroids frequetly , even in the mildest cases , my
experience is that corticosteroids topically and systemically are not
always routinely indicated in napkin dermatitis .

Fig. 176cMisuse of topical corticosteroids
(Hypopigmentation and skin rash )
I treat napkin dermatitis
as follows:
-
Wet
and macerated diaper area
I instruct the mother to
use:
Potassium permanganate
compresses 1:9000 twice daily to clean the area from debris and exudate.
Non-steroid cream,
containing mild antiseptic such as Pufexamac (Flogocid cream) is applied
after the permanganate compresses.
Gauze, either the dry one
or with olive oil or with non sensitizing antibiotic such as"
Sofratulle or Fucidin " is applied above the cream. The idea of this
is to cut short the viscous circle and prevents contact of the plastic
diaper with the infant‘s skin to minimize irritation and occlusion.
-
The dry type: gentle
cleaning of the area ,ointment such as ( Flogocid) ointment and gauze
under the diaper.
In severe dry cases:
emollient can be used and very mild steroid ointment such as( Elocom or
Eumovate ) ointment is used just for
a few days and the mother should be
instructed to stop the ointment and not to use it more than one week.
-
Secondarily infected
lesions
Topical anti-bacterial
cream such as Mupricine (Bactropan ) applied once daily and systemic antibiotic
such as erythrocin can be used.
-
Complicated lesions:
Candidiasis can be treated by mild topical preparation as " Flogocid
ointment " which is a non-steroid anti-inflammatory, antifungal and
anti-bacterial preparation. This is a safe preparation and causes rapid
clearing of the skin lesions. We found that most new born and young
children cannot tolerate the topical azoles, where the delicate and usually
abraded napkin area becomes more irritated.
N.B. : Antifungal
preparations especially those combined with steroid should be better
avoided and if there is strong indications for their use ,these should be
used cautiously and for a short period . Other Antifungal preparations may
cause severe local reaction with more erythema and irritation to the
crural areas especially antifungal lotions such as (Canstene ) . This
reaction may be due to the vehicle
causing more irritation to the macerated sensitive skin of the crural area
and the genitalia in particular .
It must be borne in mind
that the abraded skin will considerably enhance the rate of percutaneous
absorption of corticosteroid from topical application in the napkin area
or occlusive conditions found at this site.
Corticosteroid absorption
may cause hazardous side effects such as interference with the descent of
the testis especially in premature babies.
REFERENCES
-
Herpetiform napkin
dermatitis: napkin dermatitis simulating an acute herpes simplex
infection. Br J Dermatol 1986;114: 746-7.
-
Keswick BH, Seymour
JL, Milligan MC. Diaper area skin microflora of normal children and
children with atopic dermatitis. J Clin Microbiol 1987; 25: 216-21.
-
Zimmerer RE, Lawson
KD, Calvert CJ. The effects of wearing diapers on skin.Pediatr Dermatol
1986; 3: 95-101.
-
Stein H. Incidence
of diaper rash when using cloth and disposable diapers. J Pediatr 1982;
101: 720-3.
-
Buckingham KW, Berg
RW. Etiologic factors in diaper dermatitis: the role of feces. Pediatr
Dermatol 1986; 3: 107-12.
-
Jordan WE, Lawson
KD, Berg RW et al. Diaper dermatitis: frequency and severity among a
general infant population. Pediatr Dermatol 1986; 3: 198-207.
-
Munz D, Powell KR,
Pai CH. Treatment of candidal diaper dermatitis: a double blind
controlled comparison of topical nystatin with topical plus oral
nystatin. J Pediatr 1982; 101: 1022-5.
-
Berg RW, Buckingham
KW, Stewart RL. Etiologic factors in diaper dermatitis: The role of
urine. Pediatr Dermatol 1986; 3: 102-6.
-
Buckingham KW, Berg
RW. Etiologic factors in diaper dermatitis: The role of feces. Pediatr
Dermatol 1986; 3: 107-12.
-
Campbell RL,
Bartlett AV, Sarbargh FC et al. Effect of diaper types on diaper
dermatitis associated with diarrhoea and antibiotic use in children and
day-care centres. Pediatr Dermatol 1988; 5: 83-7.
-
Jordan WE, Lawson KD,
Stewart R et al. Diaper dermatitis: Frequency and severity among a general
infant population. Pediatr Dermatol 1986; 3: 198-207.
Top
|