|
SKIN MANIFESTATIONS OF INTERENAL DISEASES
|
|
|
|
The skin is a clear mirror of the human body where internal diseases may be reflected on the skin surfaces. There are different internal diseases that can cause skin manifestations . These signs may appear on the skin surface with different clinical features depending mainly on the primary internal disease: Skin color Different skin colors are associated with certain skin diseases. Pallor : as in anemia . Earthy yellowish discoloration of the skin: occurs in chronic intestinal infestations such as in bilharziasis. Plethoric: due to hyperkinetic circulation as in erythroderma and congestive heart failure. Dryness of the skin occurs in chronic debilitating diseases . Thinning of the skin: is due to exhaustion of dermal collagen such as in cachexia or locally due to topical potent steroids. Stria of the skin: occur in Cushing‘s disease, after topical and systemic steroids for a long period, dupuytren‘s contracture and in chronic liver diseases. Shape: changes in the form and shape of the skin such as moon face due systemic steroids and lymphangitis and gynecomastia that is related to increased circulating estrogens. Hair changes: fine , lanugo hair covering the skin may become pigmented as in some tumors mainly carcinomas . Hirsutism: this is caused by increased circulating androgens and cortisol due to Cushing‘s disease or systemic steroid treatment and certain ovarian tumors . Alopecia: may develop due to increased circulating androgens or changes in the sensitivity of androgen and estrogens receptors in the skin. Changes in the color of hair: metabolic and deficiency diseases such as Kwashiorkor and porphyries may cause change in the color of hair. Falling of hair: in anemia, hormonal disorders, after chemotherapy or psychic trauma . Nail changes: this occurs in chronic diseases such as pernicious anemia, liver cirrhosis leading to white bands and clubbing of nails. Xanthomatosis, acne and seborrheic like dermatitis occurs in hepatobiliary diseases. Pruritus is a common manifestation of liver diseases that is believed to be related to bile salt stasis and increase in its concentration in the blood. Cholestyramine increases fecal loss of bile salts and thus relieves itching. Edema of skin may be due to hypoalbuminaemia, increased venous pressure and increases capillary permeability. Erythroderma: erythema and exfoliation of skin may result from drug eruption and Papulosquamus diseases such as psoriasis. Urticarial lesions and alopecia areata: is related to deep psychic trauma.
SKIN MANIFESTATIONS OF LIVER DISEASES The pathological changes in the skin and its appendages in liver disease are:
SKIN MANIFESTATIONS OF RENAL DISEASES Pruritus: is a common manifestation of renal failure . The exact mechanism is not clear and may be related to secondary hyperparathyroidism that leads to mast cells proliferation. Dryness of the skin: dryness of skin in renal disease may be related to different factors mainly: Excretion of nitrogen containing compounds on to the skin surface. Decreased sebaceous gland activity leads to more dryness and also increases the viscous cycle of itching . Impaired androgen metabolism: increases dryness of the skin. This also causes fine scalp hair, with falling of axillary and pubic hair after puberty. Skin color changes: This is due to increase of melanocyte stimulating hormone occurring in chronic renal failure since the kidney is the major site of metabolism of this hormone . The skin color in renal failure varies from pallor due to anemia and hyperpigmentation due to increased melanocyte activity . SKIN MANIFESTATIONS OF ENDOCRINE DYSFUNCTIONS PITUITARY DISEASES Different skin manifestations are related to pituitary dysfunction : Acromegaly : The skin is thick due to increased collagen related to increase in circulating growth hormone leading to coarse features and tendency of keloids formation, skin tags and folds on the scalp (cutis verticis gyrata ). The skin in acromegalic patient is greasy and pigmented and covered by thick coarse dark hair. Hypopituitrism: The skin is dry, thin, atrophic leading to wrinkles, which are apparent mainly on the face with hypopigmented, faint yellowish brown patches.
The different skin manifestations are:
SKIN MANIFESTATIONS OF THYROID DYSFUNCTION Skin manifestations of Hyperthyroidism Pretibial myxedema: is the most characteristic features of thyrotoxicosis appearing as shiny waxy papules and plaques having orange-skin appearance on the chin of the tibia. Increased hair of the areas involved. Eczema : the lesions simulate atopic dermatitis in children and adults. Skin thickness: is increased leading to coarse folds which is apparent more around the eyes. The skin in myxedema appears as a coarse, dry, scaly, puffy and pale with coarse hair possibly due to increased circulating TSH. Warm skin and increased sweating due to increased basal metabolic rate. Pruritus . Hyperpigmentation or vitilligo . Premature hair graying . Alopecia and hair loss on the eye browse . The nails :become brittled and disfigured .
SKIN MANIFESTATIONS OF PARATHYROID DYSFUNCTION Hyper parathyroidism: may cause pruritus, cutaneous calcification, hemorrhage and infarction. Hypoparathyroidism: cutaneous lesions may simulate that of muco-cutanous candidiasis.
SKIN MANIFESTATIONS DUE TO ADRENAL DYSFUNCTION Skin manifestations of Addison‘s disease are due to increased melanin and androgen .These may cause different skin manifestations mainly:
Virilism Increased thickening of the skin Acniform eruption and increased seborrhea of the skin and scalp due to increased androgens .
SKIN MANIFESTATIONS DUE TO PANCREATIC DISEASES
SKIN MANIFESTATIONS OF DIABETES Skin manifestations of diabetes include the following:
5. Diabetic skin gangrene
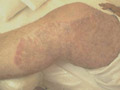
Anhidrosis: is patchy due to diabetic neuropathy leading to heat intolerance. Manifestations due to diabetes therapy Lipodystrophy: at the sites of insulin injections . Urticarial reactions due to insulin . Drug reactions: this is due to the oral medications as sulphonylureas leading to erythema multiforme and phototoxic reactions.
Fig. 353b. Drug reaction due to diabetic therapy(Sulphonylurea) Fig. 353b. Drug reaction due to diabetic therapy(Sulphonylurea)
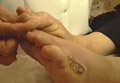
Xanthomatosis: The lesions appear in later stages of diabetics due to increased serum lipids . Trophic ulcers and bullous lesions : due to diabetic neuropathy mainly on the feet .
SKIN MANIFESTATIONS OF INTESTINAL The clinical features are due to malabsorption of the essential fatty acids. These manifestations are more common in adults than in children.
Dry scaly skin . Dermatitis herpetiformis . Fine hair . Skin pigmentation of the mucous membrane of the buccal cavity and skin creases are increased in some cases of intestinal malabsorption. Other rare manifestations: Bowel lymphoma and skin blistering due to epidermal necrosis in patients with carcinoma of the pancreas. In children, the same manifestations may appear in those fed on linoleic acid deficient diet . The common skin manifestations are: Psoriasiform rash. Dryness , cracking and fissuring of the skin. These cases improve with topical application of sunflower seed oil. Acrodermatitis enteropathica. This is a genetic disorder that may be due to zinc deficiency as in malabsorption syndrome. The condition may be fatal in infants and young children. Clinical Features. Skin lesions. Candidiasis like lesions appear on peri-oral, around the genitalia, scalp, elbows and fingers. The skin eruption is small blisters, pustules, erosions, crusting and scaling lesions. Hair and nail loss General manifestations Acrodermatitis enteropathica may be accompanied by severe diarrhea leading to cachexia. Diagnosis depends on the clinical picture and the decrease in the circulating zinc.
Intestinal malabsorption may be associated with skin and bowel vasculitis. Dermatitis herpetiformis Dermatitis herpetiformis is an immunologic problem due to deposition of IgA at the dermo epidermal junction .The condition affects all age groups but mainly in middle aged females. The skin lesion begins as a small severely pruritic papules on an erythematous base on the extensor surfaces of the limbs and trunk. Dermatitis herpetiformis is usually accompanied by coeliac disease. Eczema, scabies, erythema multiformis simulate dermatitis herpetiformis and some times it is not easy to differentiate skin lesions. The condition responds well to Dapsone and Sulphapyridine.
|
| Contents | << Previous Chapter | Next Chapter >> | Search |