|
BACTERIAL SKIN INECTIONS
|
|
|
|
PATHOLOGICAL MANIFESTATIONS
These chapters summarize briefly the most common skin infections affecting mainly infants and children. Types of Skin Infections
The skin becomes colonized by normal flora from birth. Colonization of the skin by normal skin flora is related to different factors: Age In infants and children Micrococci are more prominent than in adult‘s skin. In adults Propionibacterium are more due to the increased skin lipids. In old age streptococci and enterococci become residents of skin especially in moist areas. Sex Males carry higher numbers of bacteria than females. Race Negroes have less nasal carriage of Staphylococci than Caucasians. Type of colonizing strains Colonization of one area of skin by one strain of Staphylococci interferes with colonization by another species. Skin Conditions The skin provides a dry, mechanical barrier from which contaminating organisms on the surface are constantly removed by desquamation. Resident normal skin flora are found more on moist areas containing abundant sebaceous glands, while dry skin has less resident normal flora. Huge number of harmless normal bacterial flora colonizes the normal skin. These may be resident on the skin and its appendages or transient flora. When the immune condition is impaired or the skin is irritated or injured, non-pathogenic organisms may change their behavior and become pathogenic. The mechanism of pathogenicity and even the same strain virulence and ability to cause inflammation depend mainly on: The state of the skin epithelium and its secretions. The cellular and humoral factors. Interaction between the commensal organisms and other organisms. Permanent eradication of carriage of Staph. Aureus is not possible, but temporary elimination may be by oral or topical antibiotics but soon there will be recolonization after stopping the antibiotics.
Different species of micro flora resides normally on the skin surface without causing harmful effects under the optimum conditions of the skin. Some of this resident flora may change their behavior and become pathogenic under certain circumstances. Normal resident flora of the skin includes the following species. Aerobic Gram positive cocci: Staphylococci, Micrococci, Gram-positive rods and diphtheroids. Anaerobes Propionibacterium species: in the deeper part of the hair follicles, aerobic cocci and Pityrosporum sp. yeast present on the surface of the hair follicles and sebaceous glands. P. Acnes, P.granulosum reside on the face and upper trunk at the pubertal age, having a role in the pathogenesis of acne. Streptococcus pyogenes carriers in the throat are about 10% of the normal population, while carriers in the anterior nares are less. Natural antibiotic production by some other members of the throat flora may contribute to resistance to colonization by Strep. Pyogenes, but carriage is often not eradicated by therapeutic antibiotics. N.B.
BACTERIAL SKIN INFECTIONS Skin infections are extremely common during the neonatal period. This may be due to changes in the social and cultural behavior. Most mothers nowadays depend on housemaids or nurseries to take care of their infants or young children. This may lead to more exposure to infections and various skin diseases. Pre-school age group and young children are more exposed to bacterial infections especially the contagious ones such as impetigo. Although overcrowding, poor hygiene and existing skin disease, especially parasitic, predispose to infection, yet many cases occur in previously healthy subjects with good standard of living. Streptococci isolated from healthy individuals outside epidemics are frequently non-pathogenic but in epidemics frequently handled materials like gymnasium equipment and room dust may be important in transmitting diseases. Biting insects may transfer the disease, but in addition small non-biting flies of the genus Hippelates can contribute to the rapid spread of bacterial infections.
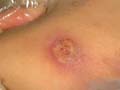
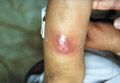
A furuncle or boil is an acute round, tender, circumscribed, perifollicular staphylococcal inflammation, which generally tends to suppurate. Furunculosis may become recurrent and constitute a problem to patients especially in the groin, nasal cavity, scalp and external auditory canal. The infection may be associated with constitutional symptoms especially in newborn and children.
Treatment General measures Preventive measures are very important especially to prevent recurrence of infection from nasal foci, autoinoculation, from perianal or intertriginous areas. This can be achieved by:
Specific measures Compresses: hot saline soaks or compresses can be applied for severe and extensive cases of folliculitis. Topical antibiotics as Muperacin (Bactroban cream), Gentamycin (Garamycin cream) or (Sodium fucidate (Fucidin cream). Topical Muperacin (Bactropan cream)applied locally once daily is also very effective and can be given alone when infection is mild, or in combination with oral antibiotics. Antibiotic orally and locally will lead usually to rapid resolution of the lesion. Oral antibiotics as (Flucoxacillin, Cephalosporin, and Cephaloridine) are effective in soft tissue infections. Erythrocin is not effective against all strains of staphylococci. Co-trimoxazole is another alternative to patients allergic to other groups. N.B.: It is of great importance not to squeeze or incise the carbuncles when they are acutely inflamed or those in the dangerous triangle of the face. If the furuncle becomes localized and shows definite fluctuation, free incision and drainage can be made.
A carbuncle is a circumscribed inflammation caused usually by Staph. Aureus complicating certain diseases such as diabetes or other conditions that lower the body resistance. Carbuncles are composed of furuncles joined together in the subcutaneous area and when sloughing shows multiple openings on the surface of the skin. Suppuration is deeply seated than in the furuncles. Clinical features Carbuncle is usually single and located most frequently on the back and lower side of the neck and on other hairy areas. The lesions manifest with painful erythema where later on localize and suppurate discharging the content on the skin surface. Sloughing leaves an irregular punched-out ulcer, which heal by scarring. Types of Carbuncles
Predisposing factors
Treatment The same treatment applied for furuncles.
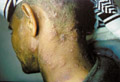
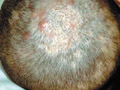
Folliculitis is bacterial infection of skin appendages that originates within the hair follicles. In infants and young children, the scalp is the commonest site involved while in adults any hairy area may be affected. Folliculitis may be superficial or deep. Superficial folliculitis: This type is also known as Bockhart impetigo that affects individuals predisposed by maceration and lack of cleanliness. The lesion begins as a small dom-shaped pustule where it may rupture, exuding yellowish exudate. The lesion in deep folliculitis is spreading deep into the follicles and causing perifolliculitis. The condition may be extensive involving a wide area especially the scalp in infants and young children and infiltrating
Impetigo is a contagious superficial bacterial skin infection most common in children caused by staphylococci and to a lesser extent by streptococci pyogenes.
Infection is usually predisposed by different factors mainly:
Impetigo contagiosa may complicate certain skin diseases such as pediculosis, scabies and eczematous eruptions. Clinical features The lesion begins usually on the face or on other areas presenting with a small reddish macule, which soon becomes a vesicle and a pustule with a thin roof that ruptures leaving an oozing abraded skin surface. Crust is formed when the lesion becomes dry. Removing of the crust leaves a smooth, moist red and oozing surface. This represents an important source of infection for others by auto-infection by the fingers or from fomites used by the patient Impetigo is highly contagious especially in infants and this is why satellite lesions appear near the primary site or on other areas due to autoinfection. Extensive lesions may involve wide areas such as the trunk and extremities, which become covered by numerous, thickly crusted dirty lesions. Severe cases may show vegetative lesions with deep ulceration. Different morphological changes may occur during the course of the disease. Some areas may show central healing while the lesions extend peripherally and join together forming annular, circinate or gyrate patterns. The lesions usually heal without atrophy or scarring.
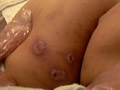
Bullous impetigo is caused by Staphylococci while, the non-bullous form may be caused by Staph. Aureus, Streptococci, or by both organisms together. The disease is usually sporadic but clusters of cases may occur in families and other groups, and larger outbreaks are occasionally seen in institutions or nurseries. Bullous impetigo occurs at all ages. In the newborn bullous impetigo may be especially widespread. This type was formerly called pemphigus neonatorum . Minor abrasions and different skin lesions may predispose to infection if the patient or a contact carries an appropriate strain of Staphylococcus . An increased incidence in hospital workers has been noted. Clinical features Clinically the disease begins as painful macule on an erythematous base, which shortly develops into vesicle or bulla and then pustule, which later on rupture exuding straw colored, sero-prulent discharge. The exudate dries to form thick infectious crust, which can cause autoinfection mainly by the fingers to the adjacent skin or to other areas of the body. When bullae are a prominent feature the designation is called ‘Bullous impetigo‘. A variety of bullous impetigo is impetigo neonatorum that occurs in the first week after birth. This type is very contagious to the maternity ward, nurses and other infants. Bullous impetigo may be accompanied by severe constitutional symptoms such as fever, diarrhea with green stool, pneumonia and nephritis. When the bulla becomes larger it ruptures leaving scalded areas of skin called in some texts as "Lyell‘s syndrome" or "Epidermal Necrolysis" endangering the life of the infant. Infection can be transmitted also through fomites used by the patient such as towels or household utensils or direct contact with the patient. The most common sites infected are the face, nasal furuncles, lips and scalp. Complications
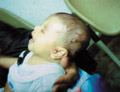
This is a highly contagious disease of the newborn infants and forms a real problem in nurseries .The disease usually manifests between the fourth and tenth day after birth , caused by Staph-aureus. Epidemics of bullous impetigo, in which some infants may develop staphylococcal scalded skin syndrome, have occurred in neonates due to transmission of infection in the nursery, principally via nursing or medical staff. Clinical features Impetigo neonatarum is a serious problem especially when there is an epidemic in nurseries. The mortality rate is high in neglected and even in treated cases. The most common sites involved are the face, perineum, per-umbilical, trunk and extremities. General manifestations Constitutional symptoms are common which include: fever, cachexia, diarrhea with green stools that may lead to severe dehydration. Bacteremia, nephritis, pneumonia, lung abscess, meningitis are severe and may be fatal complications. Skin manifestations The disease usually begins in the first or second week of life with the appearance of bullae on any part of the body, mainly on the face and extremities. Rapidly enlarging bullae with thin delicate walls and with a narrow red areola appear. The bulla has a turbid or pustular fluid. After rupture of the bulla, it leaves a denuded, oozing crusted surface. The condition may remain localized or become widespread. Differential diagnosis Pemphigus vulgaris: the bullae appear on normal skin. Nickolsky‘s sign is positive. Congenital syphilis: The bullous lesions are on the palms and soles and the presence of other manifestations of syphilis can help in the differential diagnosis. Confirmation is by serological tests for syphilis. Treatment of impetigo Preventive measures: are very important to prevent auto-infection and spread of the infection to others. Special care and special precautions in nurseries are important in order to prevent spread of infection. Specific Treatment: Drying of the exudate by potassium permanganate 1: 9000 in the form of wet compresses and application of topical anti bacterial cream such as Muperacin (Bactropan cream). Oral antibiotic such as Flucoxacillin, Amoxicillin, Cephasporin, Cefaclor and Zithromycin (Zithromax) are effective in curing skin lesions in a short time. Hospitalized cases having severe complications should be in isolated rooms and all the precautions should be considered to prevent spread of the infection to others.
STAPHYLOCOCCAL SCALDED SKIN SYNDROME The staphylococcal scalded skin syndrome is a rare acute bacterial skin infection of the newborn usually in breast-fed infants. It is caused by an epidermolytic toxin elaborated by certain strains of staphylococcus aureus, most commonly of phage group II, The organisms reach the skin, via the circulation, from a distant infective focus, usually in the middle ear, pharynx, conjunctiva or the site of circumcision or herniorrhapy. Clinical features General Manifestations The symptoms manifest with shooting fever and the infant is distressed. Recovery is usually rapid, even without antibiotic therapy. The mortality rate maybe high in certain under-developed countries. Skin Manifestations The first sign of the disease is a faint, macular, orange-red, scarlatiniform eruption occurring in association with purulent conjunctivitis or an upper respiratory tract infection. Sites of predilection are the central part of the face, the axillae and the groins. Tenderness of the skin is an early and striking feature. The presence of impetiginous crustations around the nose and mouth is rather characteristic. The eruption generally becomes more extensive, and, over the next 24-48 hours, turns to a more confluent, deep erythema with edema. The surface of the skin then becomes wrinkled before starting to separate leaving raw, red erosions. Differential diagnosis
Treatment Systemic antibiotics Culture and sensitivity may be required to detect the most effective and appropriate antibiotics. Usually Penicillinase-resistant penicillin analogue such as Flucoxacillin or Methicillin, or an appropriate Cephalosporin or Sodium fucidate are effective. If the attack is severe, the drug should initially be given intravenously. Systemic corticosteroids are absolutely contra-indicated, on the basis of experimental and clinical evidence that they aggravate the disease. Appropriate compensation must be made for heat and fluid losses. Local treatment of lesions Antiseptic baths such as 1:9000 Potassium permanganate. Antibiotic cream is then applied after drying the lesions with clean gauze. Bullae should be opened, drained and after cleaning the area, antibiotic cream and dressing can be applied. N.B. It should be noted that the disease is contagious, so all dressings or other materials coming in contact with the lesion should be burnt after use. The medical staff and other attendants should take all, the possible care and precautions not to get or transmit the infection.
Abscess is a circumscribed bacterial skin infection accompanied by local tissue destruction. Clinical features The clinical feature varies according to the causative organism and the site involved. Abscess caused by bacteria may involve the skin and internal organs. Skin and subcutaneous tissue abscess may involve the gluteal, axillary, scalp or any area of the skin. The lesion begins as an inflamed erythematous papule that is changed into a vesicle and to a pustule. The abscess is usually encapsulated and this differentiates it from other superficial bacterial skin infections such as cellulitis. The abscess may localize and has its opening on the surface of the skin exuding pus. Constitutional symptoms such as fever, headache, malaise and pain varies according to the size, site and age of the patient or any accompanying debilitating diseases. Abscess may localize in the lungs, kidneys, liver or elsewhere. The accompanying symptoms vary according to the sites involved.
Treatment Treatment of abscess depends, mainly on the causative organisms. Abscess due to bacterial infection can be treated by topical and systemic antibacterial. Opening and drainage of the abscess contents when it points to the skin. Other types of abscesses are treated according to the causative agent.
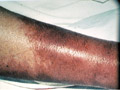
Cellulitis is a spreading infection of skin and subcutaneous tissue caused by Staph. Aureus, Strept.pyogens or Enterocococci. Trauma to the skin is usually a predisposing factor. Clinical features The skin becomes red, inflamed, swollen and tender. The inflammation is diffuse and spread to involve the dermis and subcutaneous tissue. Ulceration, lymphangitis, lymphadenitis and constitutional symptoms such as pain and fever may accompany cellulitis. The most common sites for cellulitis are the legs and face. Childhood facial cellulitis due to Haemophilus influenza is typically unilateral, and often is associated with ipsilateral otitis media. The patient presents with systemic manifestations and the affected cheek or peri-orbital tissue shows induration and discoloration, occasionally pink but characteristically purplish blue. A similar violaceous color may occur in childhood peri-orbital and buccal pneumococcal cellulitis. Treatment Severe cases of spreading infection associated with severe constitutional symptoms may need hospitalization especially if there is no response.
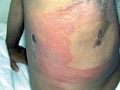
Erysipelas is an acute bacterial infection of the skin and subcutaneous tissues caused by the group beta-hemolytic Streptococci. The commonest sites involved are the face and extremities. Clinical features Prodromal symptoms High fever, chills, headache,
vomiting, and pain in the joints usually precede the onset of the
lesion. Skin lesions appear as sharply demarcated, bright red, hot skin that rapidly spread to the periphery and become pale in the center. The lesion varies from mild sharply demarcated erythema to severe inflammation and vesiculation or slight desquamation. Systemic manifestations Degeneration of the viscera due to bacterial toxins in severe cases. Vascular embolism. Serious inflammation of the internal organs of the meninges, pleura, peritoneum and synovial membranes. Septicemia and bronchopneumonia may be fatal especially in young age groups. Differential diagnosis Erysipelas has to be differentiated from:
COMPLICATIONS Local skin gangrene may complicate some cases of erysipelas where vesicles are formed first on an erythematous base that become pustular. Later on there is a blackish discoloration of the skin and severe necrosis. General Complications Severe toxemia, serous membrane inflammation, septicemia, bronchopneumonia, embolism and even death. Treatment Topical and systemic antibiotics can treat mild and localized cases. Severe cases where there is an extensive involvement of the skin or if complicated with septicemia are managed according to the severity of the case and some may need hospitalization.
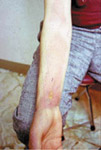
Ecthyma is a deep infection of the skin caused by beta hemolytic streptococci affecting mainly the legs. The lesion begins as a vesico-pustule, which ulcerates leaving saucer, shaped ulcer with a raw base and elevated edges. The lesion takes a long time to heal, it may take weeks or more leaving a scar. Treatment is the same as that applied for impetigo.
Listeroses is a bacterial infectious disease of man and animals. The causative organism is Leisteria monocytogens, Gram-positive microaerophilic motile bacillus found in water and soil, which is easily confused with coryneform organisms. Modes of Infection Contaminated food, especially milk, cheese and poultry, are the main source of human disease. Transplacental and birth canal infections are a well-recognized hazard to the fetus and neonate. Infection of a baby from the mother‘s milk has been reported. Some human beings may act as a carrier of the disease. Newborn infants may be infected from the infected genital tracts of their mothers. Clinical features Systemic manifestations Fever and septicemia. Granulomatous lesions may appear in infants accompanied by systemic symptoms such as carditis, encephalitis and meningitis, which may be fatal. In pregnancy, it causes a rather non-specific and generally mild, influenza-like illness in the mother, but it may lead to transplacental infection of the fetus. Severely affected babies tend to be born prematurely, and there is a high mortality rate. Skin manifestations The most common sites involved are the back and the mucous membranes of the mouth and the conjunctiva. Miliary skin lesions appear as scattered, discrete gray or white papules or pustules, about 1-2 mm in diameter, with a red margin, provide a source of organisms for culture. Purpura and morbilliform rashes may develop later along the course of the disease. Miliary granuloma, following blood-borne dissemination of infection may occur. Postmortem studies reveal miliary granulomata in many organs. The late manifestations of the disease are present with meningitis, occurring a week or two after birth. Diagnosis Diagnosis is by culturing the organism from cerebrospinal fluid and food. Biopsy from the skin and the mucous membranes. Detection of the organism in the suspected materials. Treatment Antibiotics according to the culture and sensitivity results. Combination of either Ampicillin or Penicillin and Gentamycin or Kanamycin. Topical preparations such as Potassium permanganate compress 1: 9000 and antibacterial cream. Supportive measures are very important.
Psittacosis is a human infection which is acquired from parrots (psittacoses) and other birds, e.g., domestic and sea birds. Modes of infection
Clinical features Systemic manifestations The manifestations are very variable. The incubation period is about 2 weeks. The symptoms may begin with sore throat, cough and headache. Respiratory symptoms are the most common manifestations, which vary from mild infection to severe pneumonia, cyanosis and collapse. Myocardial involvement, jaundice, encephalitis may be fatal. Skin manifestations Exanthemas occur occasionally, including a morbilliform eruption. Rose spots appear in severe cases resembling the rose spots of typhoid. Erythema nodosum was noted in some patients. Disseminated intravascular coagulation. Diagnosis Complement-fixing antibody, appearing about 10 days from the onset of infection. Isolation of the organism from lesions. Treatment Erythromycin, Zithromax is recommended for children. Tetracycline is the drug of choice in adults. Early administration is life saving. A dose of 500 mg four to six times daily usually produces a response in about 48-h and this should be continued for 10 days.
|
| Contents | << Previous Chapter | Next Chapter >> | Search |