|
BACTERIAL SKIN INECTIONS
|
|
|
|
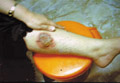
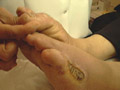
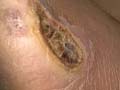
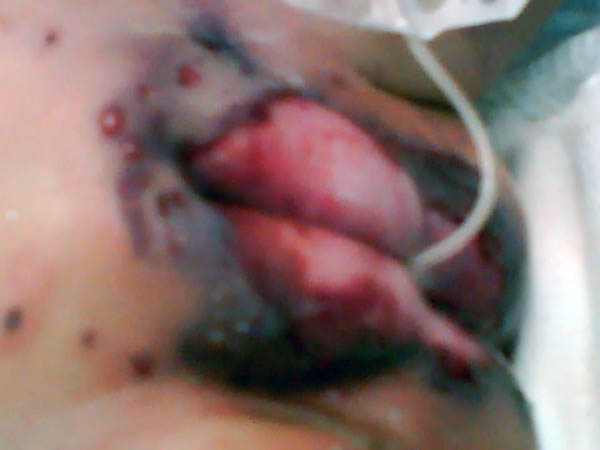
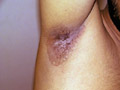
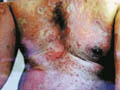
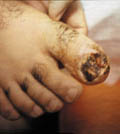
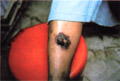
Gangrene of the skin is a serious skin problem.
Clinical manifestations General manifestations: Severe constitutional symptoms, which may lead to a fulminating course endangering life especially in young children. Skin manifestations Skin lesions may show bullae, pustules or abscesses followed by lymphangitis and lymphadenitis. After few days the skin at the inflamed site becomes dark in color, necrotic and may show extensive ulceration.
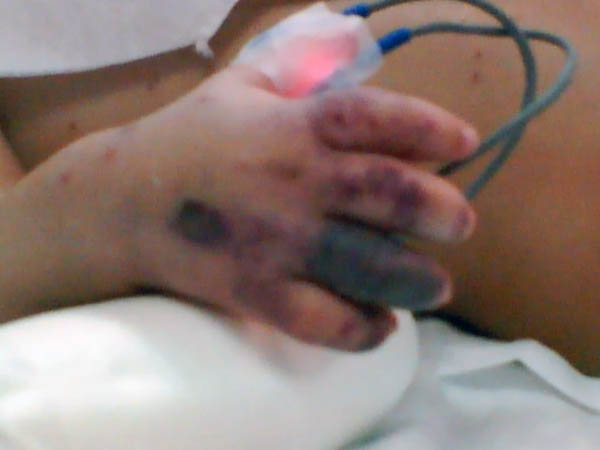
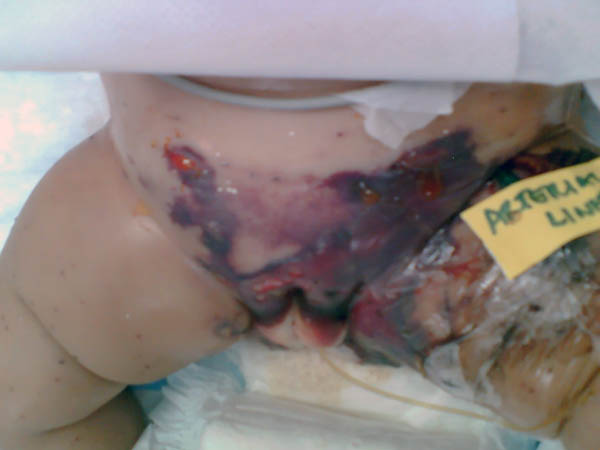
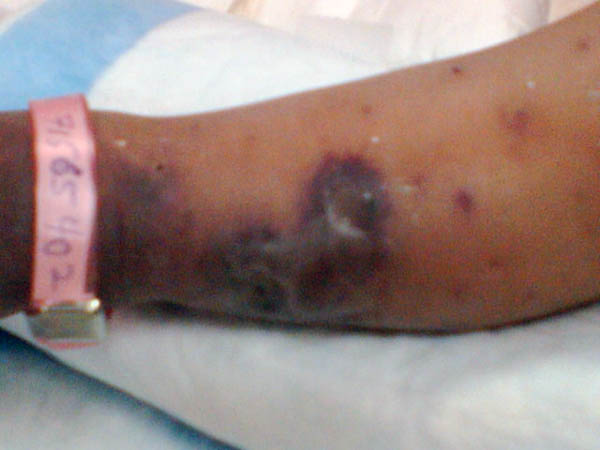
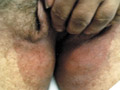
DERMATITIS GANGRENOSA INFANTUM Dermatitis gangrenosa infantum is a special type of skin gangrene that occurs in infants and young children. Two types of skin gangrene may occur in infants:
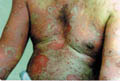
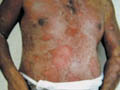
Fig.35 b,c,d,e Skin gangrene due to Chicken pox Treatment Surgical debridement and cleaning of the lesion. Cases due to Clostridium species are given gas gangrene anti serum. Wet oozing lesions can be dried by using Potassium permanganate compresses 1: 9000 followed by topical antibacterial cream as Mupricine (Bactropan). High doses of antibiotics may be needed in the beginning to control severe infection.
Erythrasma is bacterial skin infection of the intertriginous areas caused by Mycobacterium minutismus.
Characteristically, erythrasma gives a coral red fluorescence as seen under Wood‘s Light. That differentiates the condition from other crural skin diseases such as T. cruris. Treatment Mild cases can be treated by topical erythrocin lotion (Eryderm), Tolniftate, and antibacterial soap as Cidal soap. These usually can help in rapid clearance of the skin lesion. Erythrocin may be given orally for two weeks in extensive cases.
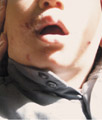
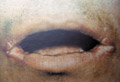
ANGULAR
CHEILITIS Perleche or angular cheilitis is a low-grade inflammation at the angles of the mouth. Angular stomatitis has been attributed to different factors:
Treatment Treatment of angular cheilitis is directed to the causative factor. Topical antifungal or anti bacterial preparations may cure some cases. Correction of the avitaminosis. Mothers should be instructed to prevent their children from licking their lips. Perfumes and perfumed soaps should be avoided. Proper mouth hygiene of the child. Pufexamac Cream or Ointment (Flogocid, Parfenac) may give good results.
Erythema Neonatorum
Exfoliativa This is a rare staphylococcal and streptococcal infection of the breast-fed infants. The disease occurs during the first weeks of life and is characterized by a fulminating course. The lesions show extensive bullous eruption with easily detached epidermis leaving red oozing areas. The condition is caused by the bacterial exotoxins. A similar condition occurs in adults known as "Lylle Disease" or epidermolysis acuta toxica. Clinical features Skin lesion presents with red macules that begin around the mouth. These change into vesicles and pustules that rupture leaving a yellowish crust. The condition may spread eccentrically to the face and other parts of the body. The skin later becomes scalded, scarlet red empetiginized, covered by vesicles and bullae. Complications Stomatitis, rhinitis and corneal ulceration. Differential diagnosis Toxic epidermal necrolysis: may simulate Ritter‘s disease. Leiner‘s disease: Leiner‘s disease shows branny greasy scales while in Ritter‘s disease there are large bullae, which peel off, in large sheets. Treatment
Toxic shock syndrome is a serious problem affecting infants and other age groups due to staphylococcal toxins. The disease is characterized by fever, multisystem involvement, circulatory shock, widespread erythema and desquamation. Clinical features The onset of the disease is acute with fever and skin rash. Constitutional manifestations: fever, vomiting, diarrhea, purpura, thrombocytopenia, alopecia and nail destruction. Systemic manifestations Involvement of muscles, liver, kidneys and central nervous system may follow. Dizziness and shock are important manifestations of the syndrome. Skin manifestations The rash may develop within the first day in the form of widespread macular erythema, papulopustular eruption or scarlatiniform that may clear within 3 days. Desquamation of the affected skin is highly characteristic. Edema of hands and feet may be marked. Towards the end of the second week the majority of patients develop a widespread, itchy, maculopapular or urticarial rash, which simulate drug reaction. Occasionally vesicles and bullae may be formed. Purpura due to thrombocytopenia may be another manifestation. Alopecia and nail changes as transverse ridging and nail loss. Mucous membrane manifestations: There is generalized mucous membrane erythema, especially intense in the conjunctiva under which there may be hemorrhage. Oral, esophageal, vaginal and bladder mucosa may ulcerate. Diagnosis The diagnosis is primarily clinical. Fever, rash, and later desquamation. Staphylococcal organisms detection from the skin or mucous membrane lesions. Bacterial culture from the primary site, not from the scalded skin, and frozen section of peeled skin may show the causative organism. Shock is a marked feature in the fully developed disease, but postural dizziness may be sufficient for the diagnosis in mild cases. Differential diagnosis
Treatment
This is a serious skin problem that may be fatal especially in infants and young children. Etiology
Clinical features Generalized skin eruption appears suddenly in infants and children following Staphylococcal infections of the upper respiratory tract. The skin shows flaccid blistering which later becomes red, scalded, tender mainly on the trunk, perioral and the peri-genital areas .The tender skin becomes gathered into folds and may separate into sheets leaving raw areas which are extremely painful. Differential diagnosis Toxic shock syndrome. Staphylococcal scalded skin syndrome. Erythema multiform and Stevens-Johnson‘s syndrome have the same clinical manifestations. Treatment Symptomatic to relieve pain and discomfort by using analgesic. Care should be taken to select an analgesic not causing drug reaction. Care of the scalded areas of skin: Potassium permanganate compresses 1:9000 and topical anti bacterial cream. Topical and systemic steroids for cases due to drug reaction. Antibiotics - culture and sensitivity to detect any causative bacteria and to be treated by the proper antibiotic (Tetracycline, Sulfa and Penicillin should be avoided because of the possibility of drug reaction.
SCARET FEVER Scarlet fever is an acute infection affecting mainly children, caused by strains of Strep. Pyogenes. Modes of Infection Droplet infection from the infected upper respiratory tract. Infected belongings of patients. From infected milk. Clinical features The incubation period is usually from 2-5 days. Constitutional symptoms Fever, which may be high, anorexia, vomiting, and sore throat. The patient is delirious or comatosed. Other serious manifestations such as myocarditis may complicate certain cases. Skin manifestations: The skin lesion appears on the second day on the upper trunk in the form of punctate erythema that becomes generalized. There is flushing of the face with pallor around the mouth, which is one of the characteristic signs of scarlet fever. Desquamation of the rash, with branny lamellar scales mainly on palms and soles. In its severe toxic form, the eruption is very intense and may be purpuric. Pastia‘s lines - Transverse red streaks appear on the skin folds due to capillary fragility. Mucous membrane manifestations: The oral mucous membranes are bright red and there may be deeper red puncta on the palate. Strawberry tongue First, the tongue becomes heavily coated. By the second or third day scattered, swollen, red papillae give the "white strawberry tongue" appearance. As the epithelium is shed the tongue becomes smooth and dark red ("red strawberry tongue"). In the septic forms the local pharyngeal lesions are severe and there may be extensive edema. Otitis media and peritonsillar abscesses are frequent. The rash may be slight. Diagnosis
Differential diagnosis
Treatment Penicillin should be given in full dose as soon as the diagnosis is suspected. Management of the complications and renal damage should be taken into consideration.
Meningococcal infection is an acute inflammation of the meninges accompanied by other systemic manifestations and skin rash. Clinical features Acute meningococcal septicemia and meningitis may present with fulminating course. Purpura follows in nearly all cases. Skin manifestations The skin eruption may be very helpful for the early diagnosis. Early skin lesions are discrete pink macules or small papular lesions that may be hemorrhagic, appearing on palms and soles. Some lesions are erythematous, morbilliform or urticarial. A purpuric eruption is characteristic, and occurs mainly on trunk and limbs. The petechiae are usually small and scanty, but vary in size and number. In severe cases larger purpuric lesions may occur including extensive ecchymoses and necrotic ulceration. The condition may be associated with a high mortality. Vasculitis may occur during the acute illness, beginning 5 -9 days after the onset even if adequate antibiotic treatment has been given. Arteritis and episcleritis may be associated with some cases.
This is a serious skin infection caused by Pseudomonas aeruginosa organisms, which is common in infants. Clinical features Skin lesions may be localized or extensive.
Complications The prognosis of systemic infections is always grave, even with early treatment. Fever and shock may supervene. High mortality rate especially in infants and young age due to septicemia is common.
This type of skin infection may be due to Pseudomonas aerogynosa organisms. Pseudomonas usually of serotype O type II, which may be cultured from the skin and the infected water. Clinical features Skin manifestations include macular, papular or pustular lesions. Some are urticarial suggesting insect bites. Any part of the body that has been immersed in water may be affected but often the worst areas are those in contact with bathing costumes. Hot tubs and whirlpools even if chlorinated may act as a source of infection.
This is a distinctive infection of the toe webs caused by pseudomonas organisms. Sharply demarcated macerated areas, sometimes tinged with green patches, characterize the lesions. The devitalized tissues are invaded by Candida albicans.
Periporitis is the term applied to pustular lesions appearing in the neonatal skin as a result of secondary infection of sweat glands by staphylococcus aureus. The commonest sites involved are the buttocks, upper part of the trunk and the scalp. The lesion affects mainly malnourished infants and young children. Skin lesions may progress to sweat gland abscesses. Sweat gland abscesses are clinically distinguished from furuncles by a lack of any tendency to "point", "coldness" and absence of tenderness. Clinical manifestations Erythematous deep seated infiltrating nodules, which may be single or multiple, small or big size. The inflammation becomes localized and soften where it ruptures exuding thick, creamy pus and later on heals leaving a scar. Differential diagnosis from furuncles can be confirmed by that furuncles arise in relation to hair follicles and have yellow center, where it points to the surface and ruptures later. Treatment Treatment is directed towards improving the nutrition and general condition of infants as well as young children. Preventing sweat retention by aeration of the crural area and minimizing sweating. Appropriate topical antibiotic may be enough to control periporitis. Oral antibiotics may be needed, especially when there are multiple abscesses.
Etiology
The organisms responsible for the infection are Streptococci group A, but also group B Streptococci, Staphylococcus aureus and Escherichia coli can cause the infection. Clinical features Skin manifestations The early skin manifestations are cellulitis, which become very indurated and extend progressively. Purpura, and occasionally bullae, may appear in the center of the indurated area, often followed by frank necrosis. Systemic manifestations The child becomes toxic. Local cutaneous anesthesia due to destruction of superficial nerves. Pneumonia. Treatment Antibiotic therapy appears to be of limited value in this potentially lethal situation. Early surgical excision of necrotic tissue is the most important aspect of treatment.
The umbilical cord may become colonized by a variety of potentially pathogenic bacteria mainly Staph, Streptococci and E. coli. Occasionally infection of the umbilical cord becomes disseminated, either by blood stream or by direct spread via the umbilical vessels to the peritoneal cavity. Tetanus, diphtheria and necrotizing fasciitis may also occur as complications of umbilical infection. Such infections are still responsible for a high proportion of deaths in the neonatal period in developing countries.
CLINICAL FEATURES Skin manifestations The skin lesion presents with cellulitis where the skin around the umbilical area becomes indurated. Bullae may appear in the center of the indurated area followed by necrosis. Purpura: Purpuric reactions are common manifestations of omphalitis and may be related to bacterial toxins.
TREATMENT The most important aspect of treatment is early surgical excision of necrotic tissue. The use of Hexachlorophene as an antiseptic was popular until it became apparent that this could lead to serious neurotoxicity, particularly in the preterm infant. The best substitute may be Chlorhexidine that can be applied as a dusting powder rather than as an alcoholic solution. Antibiotics are of limited value.
Paronychia is an inflammation of the folds of the skin surrounding the nail. Infection usually extends to the adjacent soft tissue causing painful tender swelling around the nail. Paronychia may be bacterial or fungal. Pyogenic paronychia Infection is due to Staphylococci, pseudomonas aeruginosa and less frequently to streptococci. Fungal paronychia Candida albicans is the commonest fungi causing paronychia. Dermatophytes and saprophytic fungi may be responsible for some cases of paronychia. Predisposing Factors
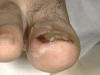
The infection is characterized by an acute or chronic purulent, tender and painful swelling of the tissue around the nail. Horizontal ridges appear at the base of the nail in chronic conditions. The moist groove of the nail and the nail fold becomes inflamed. Fig. 47b.Bacterial paronychia & Ingrowing nail
Fig.47c Bacterial Paronychia
Candidal paronychia The manifestations are less severe than the bacterial paronychia. Candida paronychia is usually chronic. The finger becomes swollen, tender and beads of pus characteristically can be squeezed from the lesion.
TREATMENT This is directed to correct the predisposing factors as preventing trauma to the fingers or toes and to keep these areas in normal dry conditions. Pyogenic paronychia Topical antibacterial and oral antibiotic besides dressing of the inflamed areas. If an abscess is formed incision and drainage is indicated. Fungal paronychia Topical and oral anti fungal medications such as Itraconazole, Ketoconazole or Fluconazole are effective. These medications should be used for a long period extending from 3-6 months.
Actinomycosis is a chronic bacterial skin infection caused by Actinomyces Israeli, characterized by suppurative granulomatous lesions with draining sinuses.
CLINICAL FEATURES The commonest sites involved are the jaw and to less extent the trunk. The lesions present with dusky red, firm, fluctuating swellings with multiple sinuses exuding yellowish granules known as "sulfur granules" which are pathogonomonic for Actinomycosis. The underlying jaw shows periosteitis and even osteomylitis. Actinomycosis is usually classified into three main types according to the areas involved.
DIAGNOSIS Examination of the granules from the draining sinuses is a characteristic of the disease. These show lobulated bodies consisting of delicate branching and intertwining filaments resembling sunrays. Gram stain of the crushed sulfur granules will show gram-positive mycelia.
TREATMENT High doses of penicillin are effective. Erythromycin and tetracycline are also effective medications.
Cutaneous diphtheria is a skin infection caused by "Corynebacterium Diphtheria." Carriers have the organism in the throat. The disease occurs in non-immunized persons with the diphtheria toxoid mainly in the tropical areas or in poor communities with poor hygiene.
CLINICAL FEATURES Different clinical pictures may be seen during the course of the disease:
DIAGNOSIS Diagnosis depends on the following:
TREATMENT Combination of diphtheria antitoxin and appropriate antibiotic. Intramuscular injection of 20,000-40,000 units of anti toxin. General measures as good supportive care, bed rest, immunization of the contacts. It should be noted that immunity requires several weeks to develop after the injection of diphtheria toxoid
Rats or other animals such as cats, or squirrels may cause cutaneous and systemic manifestations after biting human beings. Different organisms may cause different syndromes Sodoku is a clinical type caused by Spirillium minus. Haverhill Fever Septicemia caused by Sterptobacillus moniliformis due to rat bite or in some cases due to contaminated milk by the Sterptobacillus moniliformis.
CLINICAL FEATURES The clinical picture of Sodoku and Haverhill are the same and differentiation is only by the different isolated microorganism.
DIAGNOSIS Blood culture or fluid aspirated from the joints has the characteristic causative organism. Animal inoculation: Spirillium minus can be demonstrated. Blood picture - the disease is accompanied by leucocytosis and sometimes eosinophilia.
TREATMENT Penicillin is an effective antibiotic for treatment of rat bite fever. Cauterization of the wound by nitric acid may prevent spread of the disease when this is applied early after the bite.
Cat scratch disease is caused by Gram-negative rods, which are part of the normal bacterial flora of cats, dogs and some other animals. Most of the patients are children playing with cats, dogs that are a vector for the organism. Infection reaches the skin through traumatization of the skin by the cat scratch or by cat biting. General manifestations Fever, malaise and anorexia are not uncommon following the cat scratch. Central nervous system involvement. Purpura, thrombocytopenia and eye involvement are rare complications of the disease. Skin manifestations Scratch marks or bite are apparent at the site of injured skin .A red papule appears after 1-2 weeks. The papule enlarges into a nodule where the draining lymph node become enlarged, tender, suppurate and are accompanied by lymphangitis. The lesions usually heal within two weeks leaving no scarring.
Cat scratch disease must be differentiated from infectious mononucleosis, brucellosis, tularemia, histoplasmosis and sporotrichosis.
TREATMENT Usually the condition heals spontaneously. Antibiotics such as Cephalosporin, Erythrocin may give good results. Treatment of suppurating lymph nodes is by aspiration with a needle and syringe and not by incision.
Dogs are perhaps the most common assailants. They are capable of infecting soft tissue with a number of organisms that are part of normal oral flora of healthy dogs ,cats and a number of other animals. The injury varies from local wound infection to fulminate septicemia. Clinical Manifestations Skin lesions include a localized eschar at the site of the bite and cellulitis. Non-specific macular or maculopapular lesions, petechiae, purpura fulminans and symmetrical peripheral gangrene are the mainfestations. Septicemia and disseminated intravascular coagulation may occur in severe cases. Treatment Treatment of the lacerated wound. Antibiotics: Penicillin, Cephalosporin, Erythromycin, Tetracycline and Clindamycin are effective medications . Examination of the dog for the possibility of infection with rabies where that needs thorough and special treatment .
This is uncommon infection that affects mainly children. The etiology is uncertain but a necrotizing reaction due to a strain of Staph. Aureus, inoculated by minor trauma, has been suspected. The lesion is usually solitary and is often situated around the eyelids, near the mouth, or occasionally on the genitalia.
CLINICAL FEATURES Skin lesion presents with a sharply marginated ulcer, sometimes exceeding 1 cm in diameter, with an indurated base and a bright red areola that enlarges slowly after a few days. The regional lymph nodes are enlarged and tender. The ulcer may persist for several weeks before healing. It leaves a superficial scar.
DIFFERENTIAL DIAGNOSIS The disease has to be differentiated from: Epithelioma, syphilis, primary tuberculosis, accidental vaccination, swimming-pool granuloma, leishmaniasis and drug reaction. These are common dermatoses that may cause confusion in the diagnosis of chancroid pyoderma.
TREATMENT Antibiotics may improve the condition.
Pyoderma vegetans is characterized by the development of epithelial hyperplasia and chronic granulomatous changes accompanied by crusting, sinus tract formation and ulceration. Dermatitis vegetans may develop in any site but the flexures are often involved. Commonly, either Staph. Aureus or Group A streptococci are isolated from lesions but as the rash does not usually respond to antibiotics alone the role of these bacteria in the pathogenesis of the condition is unclear. Pyoderma vegetans may accompany ulcerative colitis and lymphomas.
CLINICAL FEATURES Hyperplastic and crusted plaques appear on the skin surface. These may break down and weep and there is often central clearing. When there is a prominent edge with crust formation, the lesions may mimic blastomycosis. Alternatively, there may be ulceration; the condition in this case simulates pyoderma gangrenosum. In pyodermite vegetante, crusted red plaques containing pustules have been described in multiple sites of the oral cavity, the flexures and the scalp.
DIAGNOSIS This is difficult and largely depends on the exclusion of other conditions such as specific infections, iododerma, pyoderma gangrenosum and pemphigus vegetans. It is important to exclude the underlying diseases such as ulcerative colitis, lymphoma or leukemia. In doubt, repeated biopsies from the skin lesion may be necessary.
TREATMENT Antibiotics may be of no value in controlling the condition. Application of antiseptics. Topical corticosteroids appear to produce some response. Co2 laser skin resurfacing of the lesion may be considered as one of the new methods of treatment.
Infection of the breast is common in the second or third week of life, more often in girls than boys. It is almost always unilateral.
CLINICAL FEATURES The affected breast is swollen, red, hot and tender. Systemic toxicity is usually absent. Fluctuation denotes abscess formation, which will require surgical drainage. The development of long-term breast abscess may be associated with loss of some breast tissues.
TREATMENT Hot compresses on the affected breasts Proper antibiotics Incision and drainage
Reiter‘s disease is a rare disease of unknown exact cause. Chlamydia and Mycoplasma were suspected as causative organisms. It affects mainly adult males, although it may sometimes occur in young children. The disease is characterized by triad manifestations: Non-gonococcal urethritis, Conjunctivitis and Arthritis.
CLINICAL FEATURES The disease is usually accompanied by skin and systemic manifestations. Skin manifestations Skin lesions appear as small, yellowish vesicles and ulcers. Thick, dry, horny crust may develop especially on the toes. Detachment of the crust and horny masses leaves a residual pigmentation. The sites involved are mainly, the hands, feet, genitalia, and the mucous membranes of the mouth, palate, pharynx, urethra and conjunctiva. The soles characteristically show heavy crustations and hyperkeratosis known as keratoderma blenorrhagica. Systemic manifestations Urethritis - is non-bacterial, which manifests with pyuria, and bloody discharge. Symptoms may be dysuria, stranguary, precipitancy and lower abdominal pain. Complications such as cystitis , urethral stricture , seminal vesiculitis and prostatitis may manifest with different signs and symptoms accordingly . Conjunctivitis, corneal ulcer and iritis are other manifestations. Arthritis - the onset is a sudden with pain in the heels. It may involve any joint but the knee joints are the ones commonly involved . The affected joint is swollen, tender and hot. Cardiac manifestations: Endocarditis, myocarditis, pericarditis and aortic insufficiency are rare manifestations of the syndrome. Leucocytosis and raised erythrocytic sedimentation rate are common findings.
DIFFERENTIAL DIAGNOSIS
Histopathology Epidermis - there is spongiform vesicopustules, acanthosis, parakeratosis, hyperkeratosis and elongated intrapapillary processes. Dermis - shows dilated vessels and perivascular infiltrate.
TREATMENT Rest Special care to the eye. Corticosteroids - systemic steroids and topical eye drops. Antibiotics in the form of tetracycline may have good effect. Antirheumatics and care to the affected joints.
LEPTOSPIROSIS Leptospirosis is a systemic disease that is caused by the strains of the genus Leptospira. Modes of Infection
Systemic manifestations: Sudden chills and high fever. Severe jaundice. Hemorrhagic tendency, hematuria and proteinuria. Skin manifestations Petechiae and purpura appear on the skin and mucous membranes. Severe conjunctivitis.
DIAGNOSIS Blood picture Severe leucopenia Azotaemia Blood culture: Detection of the organism. Rising of the antibodies begin in the second week. Urinalysis shows hematuria and proteinuria.
TREATMENT Symptomatic Antibiotics such as Tetracycline and Chloramphenicol may be of value in the adult age. Children may be given erythromycin or zithromax
|
| Contents | << Previous Chapter | Next Chapter >> | Search |