|
VESICULO-BULLOUS
DISEASES
|
|
|
|
Certain drugs can induce pemphigus - like reaction.
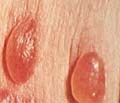
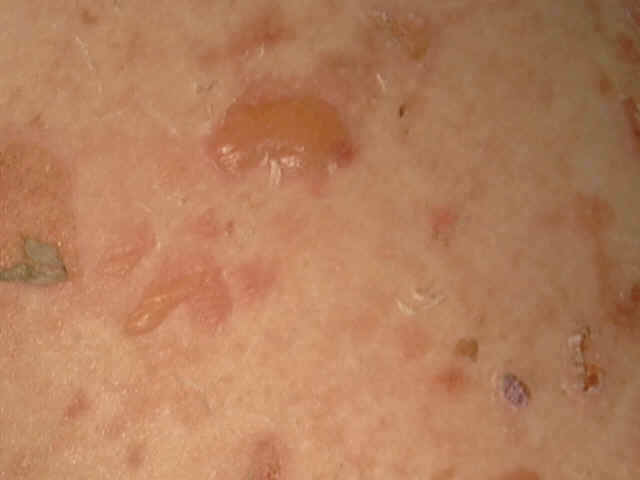
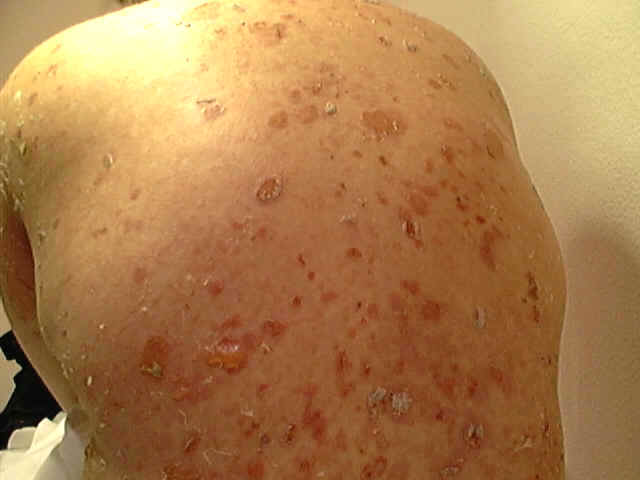
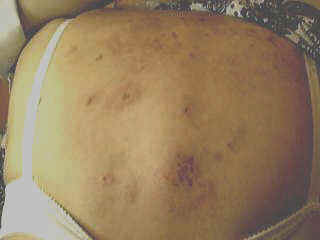
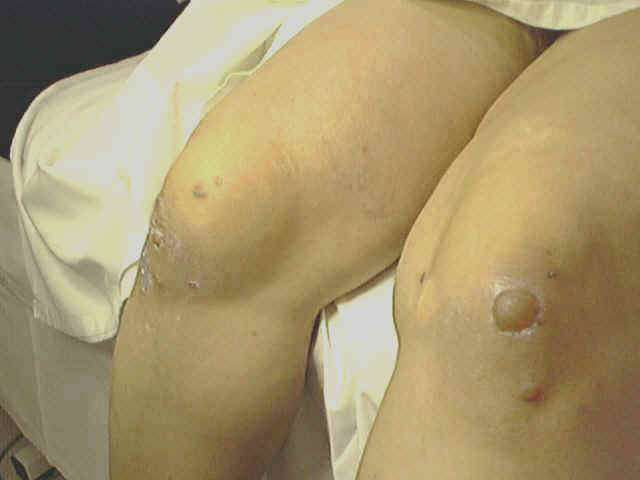
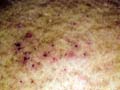
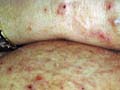
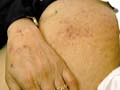
Pemphigus vulgaris is a rare relapsing disease affecting skin and mucous membranes. Clinical Features. The disease is characterized by flaccid bullae, which appear on normal or erythematous skin surface. The bullae may appear in waves, grouped or annular and are filled with serosanguinous, sero-prulent or hemorrhagic exudates. Fig. 283:1-8: Different clinical types of Pemphigus Vulgaris Fig. 283 Pemphigus vulgaris Fig. 283. Pemphigus vulgaris (Flaccid Bullae)
Fig.283-1 Pemphigus (Nicoklysk's signe +ve) Fig. 283-2 Pemphigus vulgaris(infected bullae)
Fig.283 Pemphigus vulgaris
Fig.283-4 Pemphigus-Subungual bullae
Fig. 283-5 Pemphigus vulgaris Fig.283-2 Pemphigus of the scalp and cicatricial alopecia
Fig.284. Pemphigus vulgaris
Fig. 286 d,e,f - Pemhigus vulgharis
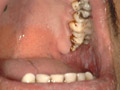
Nickolsky‘s sign is characteristic for pemphigus. This test can be performed by drawing of the finger with firm pressure over the surface of the skin covering the bulla which is apparently normal , shows that the epidermis slides off much like a piece of wet tissue paper. The sites involved are usually the areas subjected to pressure or rubbing and the mucous membrane of the mouth and larynx Symptoms at the beginning are minimal such as mild itching or burning of the areas involved. The bullae rupture on the skin and mucous membrane leaving denuded eroded painful surface. Secondary bacterial infection is common where healing takes longer time. Healing usually leaves residual hyperpigmentation but without scarring.
Pemphigus vulgaris is unusual in pregnancy. Several cases were shown to be transmitted via the placenta. Affected infants may have cutaneous and/or mucosal erosions or bullae, where others were stillborn. Diagnosis of Pemphigus Vulgaris
Pemphigus vegetans is characterized by hypertrophic vegetations formed after rupture of the bullae mainly on the intertriginous areas. Clinical Features The vesicles affect first the oral cavity and then spread to cover extensive areas of the skin. Secondary bacterial infection is common which may lead to constitutional symptoms, malodorous smell of the mucous membrane, and skin lesions. Differential Diagnosis of Pemphigus
Pemphigus folacious is a rare bullous disease involving an extensive area of the skin, usually in the form of exfoliative dermatitis. Clinical Features Skin lesions begin as small vesicles that gradually exfoliate and become crusted covering wide areas of the skin. The condition at this stage is not easily differentiated from exfoliative dermatitis. The lesions of pemphigus folacious have symmetrical distribution.
Fig.285b. Pemphigus folacious Fig. 285c. Pemphigus folaciousFig.285b. Pemphigus folacious Itching is minimal but secondary bacterial infections are common. Nails and hair usually fall.
Brazilian pemphigus has the same cutaneous manifestations of pemphigus folacious and the difference depends on age and time of onset. This type begins in younger age groups and is accompanied by endocrine disturbances. The lesions begin on the face (butterfly area) and chest in the form of erythematous scaly, crusted lesions, simulating lesions of seborrheic dermatitis and lupus erythematosus.
Fig. 285b.Pemphigus erythematosus Histopathology of Pemphigus Acantholysis is the degeneration of the intercellular bridges Hyperkeratosis. Spongiosis. Epidermal eosinophilic microabscesses with intra-epidermal cleavage. The dermis shows mild inflammatory infiltration by lymphocytes, eosinophils and plasma cells. Treatment of Pemphigus
BENIGN
FAMILIAL CHRONIC PEMPHIGUS Benign familial chronic pemphigus is a rare hereditary disease unrelated to pemphigus vulgaris although they have the same histopathological picture. Clinical Features Lesions develop mainly in areas exposed to friction, such as the sides of the neck, axillae and groin, but less commonly involve the scalp or extremities. Skin lesions are characterized by recurrent eruptions of flaccid vesicles with clear or turbid fluid on normal or erythematous skin. Lesions extend peripherally and the center may heal or show soft, flat, moist vegetations. Spontaneous remissions occur in cold weather and most patients find that heat and sweating aggravate the condition. Mucous membrane lesions are un common. Differential Diagnosis Candidiasis T. Cruris Pemphigus vegetans of the crural areas. Darrier‘s disease. Treatment Antibiotics: Hailey -Hailey disease characteristically responds to antibiotics locally and systemically. Anti fungal preparations can be given when fungal lesions are detected. Topical steroids in combination with antibacterial or anti fungal topically (Decoderm trivalent, Lotriderm, Kenacomb) may cause clearance of the skin lesions. Systemic steroids are rarely indicated in contrast to pemphigus, where systemic steroids are considered the main line of treatment.
This is an auto-immune blistering disease which is rare in childhood. Bullous pemphigoid is characterized by accumulation of IgG antibodies at the dermo-epidermal junction in a linear band.
Localized mucosal pemphigoid. Fig. 286.a,b,c. Bullous pemphigoides
Some types of bullous pemphigoides are associated with malignancy. Clinical Features.
Treatment The same lines applied for pemphigus. Corticosteroids and immunosuppressive drugs may be an effective treatment.
BULLOUS
PEMHYGOID OF CHILDHOOD Chronic bullous disease of childhood is rare. Different nominations were given for this disease such as: Bullous pemphigoid of childhood, juvenile dermatitis herpetiformis, juvenile pemphigoid and childhood bullous dermatitis herpetiformis. Clinical Features Large blisters develop, which may become very extensive, involving usually the genitalia, buttocks and inner thighs. Most patients have the lesions on the scalp, peri-oral area and to a lesser extent on the mouth. Large clear bullae predominate but are occasionally haemorrhagic, and usually arise on previously normal skin. Only rarely the lesions manifest with wheals and papules. New bullae may cluster around an older lesion forming a so-called ‘cluster of jewels‘. Healing is rapid with hyperpigmentation but generally without scars. The vesicles and bullae are moderately pruritic, predominantly over the pelvic and peri-oral regions. The eyes are often sore or gritty and rarely there is conjunctival scarring. Differential Diagnosis Bullous impetigo: bullous impetigo may resemble the initial lesions of childhood bullous pemphigoid, but its short duration and response to antibiotics can help in the differentiation. Epidermolysis bullosa: are often present at birth and the lesions when heal leave scarring of the skin and mucous membrane. Incontinentia pigmenti and Acrodermatitis enteropathica may cause confusion, but the onset of bullae within the first few weeks of life in the former and the mucous membrane lesions of the latter should help to differentiate both diseases. Bullous papular urticaria: rarely affects the face or genital region and usually has short duration. Pemphigus: pemphigus is rare in childhood and the diagnosis depends on the clinical picture, histological and immunological manifestations. Pemphigoid may give a similar clinical picture, but the deposition of IgG and C3 at the basement membrane zone is usually diagnostic.
Dermatitis herpetiformis is a pruritic blistering skin disease, occasionally seen in children. The disease has an immune origin and may be accompanied by coeliac disease. Severe emotional stress may act as a precipitating factor. Clinical Features Skin lesion begins as excoriated pruritic erythematous papules, urticarial wheals or a grouped small vesicles or bullae. The lesions appear on the extensor aspects of the limbs, especially the knees, below the elbows, axilla, trunk, shoulders, face and scalp. In late stage the lesion may present with pigmentation and grouped scars. Oral lesions are not uncommon. Progressive pigmentation of the sites of the skin lesions occurs in half of the patients. Dermatitis herpetiformis may be associated with gastro-intestinal enteropathy presenting with a clinical picture of coeliac disease. In children dermatitis herpetiformis often involves the genitalia, sacral, axillary folds, buttocks and extensor surface of the limbs. In children the disease is usually asymptomatic, more common in male children and curiously the disease in young age groups does not respond to sulfapyridine and other medications that are effective in the adults. Dermatitis herpetiformis may begin in childhood as papulovesicular or bullous lesions that may extend to the adulthool which show exacerbation and remission course. Dermatitis herpetiformis by immuno-phlorescence shows IgA antibodies accumulation at the dermo-epidermal junction. Differential Diagnosis The symetrical distribution, grouping of lesions, severe pruritus, configuration with different shapes and response to sulphapyridine and dapsone can differentiate the disease. Histopathology Edema of the tips of dermal papillae and infiltration with neutrophils and eosinophils. Subepidermal separation. Bulla formation. Degeneration of the tips of the papillae. Separation of the epidermis and the confluence of several dermal tips produce vesicles. Treatment
Dosage of Dapsone The adult dose as a starting dose is: 50-100 mgm. /day. The dose may be increased to 400 mgm /day according to the patients response then a maintenance dose of 25 mgm/ week can be recommended. Many patients with dermatitis herpetiformis can be controlled on lower doses. Toxicity Toxicity of Dapsone is a big problem but overall the drug has probably fewer long-term side effects than do corticosteroids or Sulphapyridine. The commonest side effects of Dapsone are: Haemolysis Methaemoglobinaemia This is also common and is responsible for the bluish lips. Regular blood checks of hemoglobin and reticulocytes but also including white cells and platelets should therefore be undertaken in all patients for the first few months after starting Dapsone. Bone-marrow damage. Peripheral neuropathy. Drug rashes Renal damage Hypoalbuminaemia Cholestasis Psychoses Reversible male infertility.
SUBCORNEAL PUSTULAR DERMATOSIS Subcorneal pustular dermatoses is not related to infection where micro-organisms could not be cultured from fresh lesions, meanwhile IgA and IgG immunoglobulins have been detected. Subcorneal pustular dermatosis is affecting mainly old women. In younger patients the general health is not affected but myeloma may be seen in old age groups. The most common sites involved are the flexor surfaces of the limbs, axilla, submammary areas and the groin. The disease has a chronic benign, relapsing course and the pustular eruption has the distinctive histology of a subcorneal bulla containing neutrophils. Clinical Features The lesions of subcorneal pustular dermatosis are characterized by: Transient grouped vesicles that soon become pustular having different shapes; annular, gyrate or spread peripherally with a serpiginous edges. The pustules rupture leaving superficial leafy scales and faint brown-pigmented area. The eruption may appear in successive waves in the same areas after healing. Differential Diagnosis Impetigo Can be easily distinguished by the presence of pathogenic organisms and the response of the lesions to antibiotics. Dermatitis herpetiformis Can be differentiated by the clinical, immunological features and its response to Dapsone and Sulphapyridine. IgA immunoglobulins can be detected in dermatitis herpetiformis, characteristically both in the region of the blister and in normal skin. Pemphigus foliaceus May show an intra-epidermal bulla without acantholysis and may even respond to Dapsone, but has characteristic direct immune-fluorescence. Eosinophilic spongiosis Differentiated by the clinical pattern and the positive direct immuno-fluorescence, but repeated biopsies may be needed to obtain the typical spongiotic histology. Pustular psoriasis : may resemble subcorneal pustular dermatosis very closely, either of the acute von Zumbusch type with small pustules, or the spreading annular type. However, the natural history of the disease, the response to Dapsone and the fact that the subcorneal pustule sits on the surface of the epidermis rather than being an integral part of it serves to distinguish the two conditions. Chronic benign bullous disease of childhood can produce a subcorneal pustule, as can a number of other disorders. Erythema multiform The distribution, symmetry, tendency to iris formation and bulla formation are characteristic. Pustular bacterid A generalized pustular eruption following an upper respiratory infection described as a pustular bacterid occasionally shows subcorneal pustules. Treatment of Subcorneal Pustular Dermatosis. Local treatment General hygiene to the abraded skin surfaces. Drying lotions such as potassium permanganate 1: 9000. Vitamin A cream may have some effect. Topical steroids are usually not helpful. Systemic treatment Dapsone is the drug of choice that can give good results without relapsing after stopping treatment as in dermatitis herpetiformis. Dapsone dose is 50-150 mgm / day for adults. The dose is usually monitored according to weight, age and the severity of the disease.
|
| Contents | << Previous Chapter | Next Chapter >> | Search |