|
DISEASES OF THE SWEAT GLANDS
|
|
|
Alteration in the function of sweat glands is either : Increased sweating: hyperhidrosis Decreased sweating: anhidrosis due to sweat retention or limitation of sweat production .
Hyperhidrosis is an abnormal increase in the amount of sweat. These may be related to different factors, which may be physiological or pathological. Hyperhidrosis may be generalized or localized involving mainly palms, soles and axilla. Generalised hyperhidrosis Different factors can affect the eccrine sweat glands and increase their sweat production:
Localized hyperhidrosis: Localized hyperhidrosis is a very common condition causing in certain instances a psychological, occupational and social problem especially when different lines of treatment fail to control this condition. Etiology Emotional hyperhidrosis: Any age and sex may have this problem. It may be very localized involving the palms soles or extend more to involve the axilla, crural areas or the waist where profuse sweating occurs when the patients are exposed to certain stimuli. Familial factors Neurogenic factors Increase of the activity of the sympathetic nervous system such as in hyperactive children, emotional imbalance, vasomotor instability all may cause increase in sweating. Physical factors Different factors may trigger the condition such as pain, mental stress, fear, and physical effort. Treatment of Hyperhidrosis Patient reassurance and psychotherapy may help some cases especially the emotional type. Anticholinergic drugs Sedatives: Benadryl or other types of mild sedatives improve hyperhidrosis. Synthetic analogues of atropine such as Banthin and Probanthin have temporary inhibitory effect of sweat .The side effects as some patients may not easily accept, are dryness of mouth, blurring of vision with higher doses. Antihistamine: Cyproheptadine or Citrizine may be of value in treatment of hyperhidrosis, especially the emotional type. Topical preparations: Many topical preparations are available in the market but some may cause contact dermatitis besides plugging of the sweat ducts orifices, causing anhidrosis, sweat retention and hidradenitis suppurativa. Most antiperspirants contain aluminum salts in different concentrations and combinations. Astringents: Palm and foot soaks with: Potassium permanganate 1: 2000 , 2 per cent Burrows solution and tannic acid in alcohol for an hour may have antiperspirant effect. Powders: These are used for dusting of the feet and the interdigital spaces to minimize sweating. The commonly used powders are: R/x
This preparation may have a good effect in decreasing localized hyperhidrosis. Botulinum toxins Recently botulinum toxins proved to be effective, safe and long lasting alternative therapeutic modality for treatment of severe palmer hyperhidrosis. Method The patient is given 50 subcutaneous injections, 2 mouse units each in each palm using regional nerve blocks of the median and ulnar nerves. Aluminum-chloride hexahydrate 25% in absolute ethanol can give effect in axillary hyperhidrosis. Iontophoresis Tap water Iontophoresis is a recognized method of reducing sweat in various parts of the body. Ionotophoresis, the process of increasing the penetration of drugs into surface tissues by the application of an electric current. The drionic device is a battery-operated method of inducing tap water Ionotophoresis. This simple device may be used at home and is effective in reducing hyperhidrosis for as long as 6 weeks.
Malodorous sweat may occur in the axilla and feet. In most cases it is associated with: Hyperhidrosis Apocrine glands dysfunction Bacterial and fungal infections Fatty acids decomposition producing distinctive odor. Certain foodstuffs such as garlic, onion and excessive protein ingestion. Heavy metals: arsenic. Treatment Treatment of the cause if possible. General cleaning of the body and frequent bathing. Changing of socks and under wears repeatedly and using light clothes. Avoid excess sweating. Avoid certain types of food such as excess proteins, garlic, and spices. Aeration of the area . Dusting powders especially for the feet before dressing the socks. Soaks for the feet such as potassium permanganate 1: 2000 or formaldehyde solution. Deodorants: are available in different preparations. Care of local sensitization due to certain products. Antibacterial antiseptic soap (Cidal soap)
Chromohidrosis is colored sweat due to dysfunction of the apocrine glands. The commonest site is the face, where the color of sweat may be black, green, blue or yellow. The crural areas may be involved where a rusty stain may appear on the underwear.
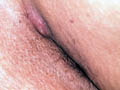
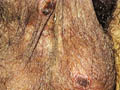
Hidradenitis suppurativa is infection of the apocrine sweat glands mainly that of the axilla and the inguinal areas. Tender reddish nodule appears, firm that may cause an abscess with multiple openings on the skin surface and discharging pus. The condition is chronic and has the tendency of recurrence. Scarring may accompany severe cases. Treatment Local compresses with potassium permanganate for oozing cases and topical antibiotics.
Fox Fordyce disease is a rare disease occurs mainly in young girls not before puberty and not after menopause. Clinical Features Intense pruritic, small, flesh colored papules occur mainly on the axilla, mamma, umbilicus, perineum, labia and rarely in males on the scrotum. The papules may increase in size forming nodules with an empty follicular center.
Treatment Treatment of the disease is not always successful. Estrogens and contraceptive pills have been used. These may give improvement to itching and involution to the lesions.
POMPHOLYX Pompholyx is a vesicular eruption of the palms and soles .The vesicles are deep and appear as sago grains filled with clear fluid mainly bilateral around the fingers and toes. The symptoms are minimal where there may be mild itching or burning of the sites involved. The lesions may be grouped. The disease was discussed in previous chapters in dyshidrotic eczema. Etiology Hyperhidrosis Emotional stress Contact dermatitis Drug allergy Food allergy: spicy foods or the additives in food. Bacterial and fungal infection else where in the body as an allergic or id reaction. Treatment Treatment of the cause such as hyperhidrosis or infections. Potassium permanganate 1: 8000 soaks are effective for the hands and feet. Topical corticosteroids cream alone or in combination with antibacterial preparation (Decoderm compound).
MULTIPLE SWEAT GLAND ABSCESSES This disease affects mainly young infants .The causative organisms are usually Staph.pyogens. Clinical Features Multiple dome -shape, non-tender and non-pointing abscesses affecting mainly the scalp, trunk and buttocks. The lesion may form boggy; fluctuating dome shaped swelling that ruptures spontaneously. Treatment Potassium permenganate compresses. Topical antibacterial cream such as muperacin (Bactroban cream) Systemic antibiotics. Incison and drainage.
Anhidrosis means absence of sweating. Anhidrosis is the absence of sweat due to defect in production or conduction of sweat to the skin surface in the presence of an appropriate stimulus. The condition may be localized or generalized. Types of anhidrosis Generalised anhidrosis: Causes of generalized hyperhidrosis Miliaria Congenital ectodermal defects Orthostatic hypotension Diabetic neuropathy Multiple myeloma Thyrotoxicosis Myxedema Pemphigus Segmented type of anhidrosis This type occurs in: Horner‘s syndrome. Multiple sclerosis. Etiology New born and premature infants commonly show temporary anhidrosis for several weeks probably due to immaturity of neural supply. Neural causes: Head injuries, heat stroke, hysteria, and neurosurgical problems. Operations: tumors in the region of the third ventricle leading to loss of control of the thermoregulatory centers in the hypothalamus. Occlusion of the sweat ducts or their pores lead to sweat retention anhidrosis as in miliaria, contact dermatitis, atopic dermatitis, icthyosis and psoriasis. Topical antiperspirants containing aluminum sulfate. This type of anhidrosis is the most common seen in general practice. Post ganglion sympathectomy lead to anhidrosis in the areas supplied by these fibers. Degeneration of the peripheral sympathetic fibers as in peripheral neuritis and diabetes. Drugs: anti cholenergic drugs, atropine and its analogues and local anesthetics. Congenital absence of the sweat glands, either in localized areas or generalized as in congenital ectodermal defect, which is hereditary, transmitted as sex - linked recessive trait. Atrophy of sweat glands as in burns, radiodermatitis and accompanying certain diseases such as scleroderma and exfoliative dermatitis. Idiopathic Treatment Treatment of anhidrosis is usually not successful without the control of the causative factor. Treatment of the complications due to sweat retention such as miliaria. General measures: Avoid vigorous exercise Avoid exposure to hot environment. Air-condition and humidifiers may help the patients.
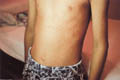
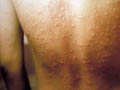
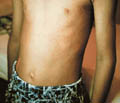
Sweat retention in children and older age groups may have different predisposing factors and some variations in the clinical features. The condition is due to interference in free delivery of sweat to the skin surface. Occlusion of the sweat ducts pores by keratin in response to epidermal injury may lead to rupture of the sweat glands. The condition is called miliaria or sweat retention. Clinical Features - Sweat retention anhidrosis: due to poral occlusion only causes minimal symptoms apart from anhidrosis. - Miliaria group: Different types of miliaria have different clinical symptoms and signs. Miliaria crystallina This is due to escape of sweat in the stratum corneum leading to numerous discrete vesicles with clear fluid, which ruptures easily. Symptoms are usually negligible where some cases have little burning or stinging sensation when exposed to strenuous effort or in hot humid environment. Miliaria crystallina may be found in association of contact dermatitis especially in young children due to occlusion of the crural area for long time or using powders, which may occlude the sweat orifices. Miliaria rubra or prickly heat: This is the most common, especially in hot humid climates appearing on the back, chest, side of the abdomen, antecubital, popliteal fossa and in areas exposed to friction. The lesion manifests as erythematous papulovesicular rash causing itching and burning sensation due to leakage of sweat into the epidermis, where the severity depends on the heat load. Miliaria pustulosa: The lesions appear as pruritic, discrete, superficial erythematous pustules with a dark punctum at the center corresponding to the hyperkeratotic plug occluding the sweat orifice. The common site of miliaria pustulosa is the intertriginous areas and the flexural surfaces of the extremities. This type is also common in young children using diapers and associated with certain diseases as intertrigo, atopic dermatitis and contact dermatitis. The contents of the pustules are sterile and it is formed due to intraepidermal sweat retention. Miliaria profunda: This type is due to deep poral occlusion and rupture of sweat ducts and escape of sweat into the epidermis at the dermo-epidermal junction. Clinical Features The skin eruption is in the form of non-inflammatory, non-pruritic and flesh colored papules where the severity of the lesion depends on the degree of sweating. Miliaria profunda may be accompanied by systemic manifestations such as irritability, easily fatigue ; headache, anorexia, drowsiness and inability to concentrate due to heat intolerance. Miliaria improves by cooling of the skin and the symptoms may disappear after a short time. Miliaria in infants Miliaria occurs when the flow of eccrine sweat is impeded by obstruction of the intraepidermal portion of the sweat duct. Relative immaturity of the sweat ducts may be an important predisposing factor in early infancy. Occlusive pants provide favorable conditions for the development of miliaria in the napkin area.
DISEASES OF THE APOCRINE GLANDS Apocrine glands are not active in childhood and smaller in size. Their activity is related to sex hormones and has no heat regulatory role as that of the eccrine sweat glands. Apocrine glands are present in special areas of the body such as the axilla, nipple, face, pubic area and genitalia. Secretion of apocrine glands is small in amount odorless but give distinct odor under certain conditions due to action of bacteria liberating unsaturated fatty acids, which give the characteristic aromatic odor. The odor varies according to the age, sex, race and emotional status of individuals. Infection of the apocrine glands is mainly in the axilla and called hidradenitis suppurativa. Occlusion of their pores leads to cyst formation or papular, itchy and intensely pruritic eruption called Fox -Fordyce disease. Treatment The effective treatment includes decrease the secretion by aluminum salts and inhibits bacteria in the area by shaving the hair in adults which invites debris, bacteria besides keratin and repeated cleaning the areas with water and soap. Topical and systemic antibiotics.
|
| Contents | << Previous Chapter | Next Chapter >> | Search |